 View / Download pdf version of this article
View / Download pdf version of this article
Nationally Funded Modules available for general practice
BPAC Inc is pleased to be able to offer general practices a suite of clinical decision support modules, free-of-charge.
These modules have been nationally funded for healthcare professionals in New Zealand through arrangements with the Ministry
of Health, PHARMAC and Medsafe.
These modules act as a both a decision support tool and process guide in each clinical area. Individualised options,
questionnaires, standard treatment suggestions and appropriate referral documents are generated in a logical flow. Links
to relevant websites for additional information and support are built in to each module. Downloadable patient information
and/or links to suitable online patient advice are at your immediate call.
The Nationally Funded modules are accessed via Best Practice decision support, which can be installed free-of-charge
at any general practice in New Zealand.
The Nationally Funded suite is made up of the following modules:
- Adverse Reaction Reporting
- Hazardous Substances & Lead Poisoning Notifications
- Childhood Asthma
- Childhood Asthma – Action Plan
- Depression (4 modules)
- Depression in Adults
- Depression in Young People
- Ante/Postnatal Depression
- Depression in the Elderly
- INR
- Acne Management
- Isotretinoin
- TIA/Stroke – recently released nationally
- Chronic kidney disease – coming soon
Adverse Reaction Reporting
For the last two decades or more, New Zealand has had one of the highest rates per capita in the world of reporting
adverse reactions to medicines. This high rate does not, however, reflect a more serious problem in New Zealand with adverse
reactions to medicines; rather that we are more diligent about reporting these events.
To help maintain this trend, this module enables the reporting of suspected adverse drug reactions directly to the National
Centre for Adverse Reactions Monitoring (CARM). By “auto-filling” with information already held in the Patient Management
System (PMS) the reporting of an adverse reaction is rapid and efficient. A copy of the report is automatically saved
on the patients’ record.
Hazardous Substances & Lead Poisoning Notifications
General Practitioners are now asked to notify cases of disease and injury caused by hazardous substances seen in primary
care to their appropriate Medical Officer of Health. Notification may result in a Public Health Unit investigation of
that particular event or a collection of related cases, or may initiate the investigation of a particular substance in
a region or nationwide. This module guides the user quickly through the reporting process, supplies the information needed
by the Ministry of Health and forwards the notification to the appropriate recipient. A copy of the report is then automatically
saved to the patients’ record.
Childhood Asthma
New Zealand has one of the highest rates of childhood asthma in the developed world. Between 20 – 30% of the children
in your practice are predicted to develop symptoms. Based on current guidelines, this module provides decision support
for the diagnosis, control and treatment of childhood asthma using a stepwise approach. This in turn links into the Childhood
Asthma Action Plan module.
Childhood Asthma – Action Plan
This module enables you to create an individualised action plan for a child with asthma (Space-to-Breath), illustrating
which device they should use and when to use it. A black and white copy can be given to the family at the consultation
and a high quality, colour version is automatically generated and posted to the patient’s address.
Depression
The World Health Organisation estimates that by the year 2020, depression will be the second most common cause of ill
health and premature death worldwide. The depression modules are divided into four key groups of patients: Young People,
Adults, Elderly People and Ante/Postnatal depression. The patient’s demographic information is used to initiate the appropriate
module, with relevant questionnaires and tools.
These modules allow you to step through the appropriate questions as you talk with your patient, giving you more time
to listen and engage. This is followed by the guidelines which suggest appropriate treatment and /or referrals. Patient
resources, including further questionnaires, information and website links, are included in the modules.
Young People
Every interaction with a young person in primary care should be regarded as an opportunity to assess their psychosocial
as well as physical wellbeing. Young people may not be forthcoming with their problems and issues, but sensitive questioning
can identify the need for further assessment.
Adolescent depression is similar to depression in adults, with a greater likelihood of mood symptoms at presentation,
but these may still be masked by behavioural problems, substance misuse or somatic symptoms. The assessment tools within
this module will assist and support you as you work with these young patients.
Adults
People are reluctant to discuss their depression symptoms for a number of reasons. It is estimated that two-thirds of
people with depression who see a healthcare provider present with physical symptoms, such as headache, back problems or
chronic pain. Use of this module during a routine consultation will help clarify and quantify a diagnosis of depression
and subsequent management plan.
Ante/Postnatal
Depression affects up to 10% of pregnant women and up to 15% of women in the postnatal period. This module focuses on
the recognition, assessment and management of patients during this important time in their lives.
Elderly people
Many older people are reluctant to “bother” their general practitioner about something other than a physical illness.
They seldom mention depression and are more likely to talk about vague symptoms. Although they know they need help, some
people have difficulty putting troubled feelings into words. Many older people may also perceive that a low mood is normal.
Tools within this module, such as the Geriatric Depression Scale, have been specifically developed for older populations
to help address these issues and to give more weight to mood related symptoms.
INR
There are approximately 46,000 people in New Zealand currently taking warfarin. This module utilises a validated formula
to assist in ongoing management of a patient’s anticoagulant dosing. Included is a review page which prints back to your
PMS, graphical display of INR level history, a calculator for average dose rate and a printable calendar for the patient’s
use which clearly shows their daily dose regimen.
Acne Management
Acne is one of the most common skin conditions, affecting up to 80% of people aged between 15 to 25 years. This module
assists you in assessing the severity of acne, and directs you to the most appropriate resources and treatments options
for your patient. If isotretinoin is an appropriate treatment, you can progress seamlessly to the isotretinoin module
to initiate and manage this.
Isotretinoin
This module can be used either as a stand-alone module or as part of the acne management module; progress through patient
consent documents, laboratory request forms, results and writing of the prescription, with quick access to the Special
Authority process. This module is designed to meet the PHARMAC recommendation that a support tool be utilised when prescribing
isotretinoin. Both patient and prescriber information about the safe use of isotretinoin are included.
New modules: TIA/Stroke and Chronic Kidney Disease
The Ministry of Health has now funded two new Best Practice modules for national release – TIA/Stroke assessment and
Chronic Kidney Disease. These modules will be rolled out to practices over the coming months. Further information will
be provided in the next update.
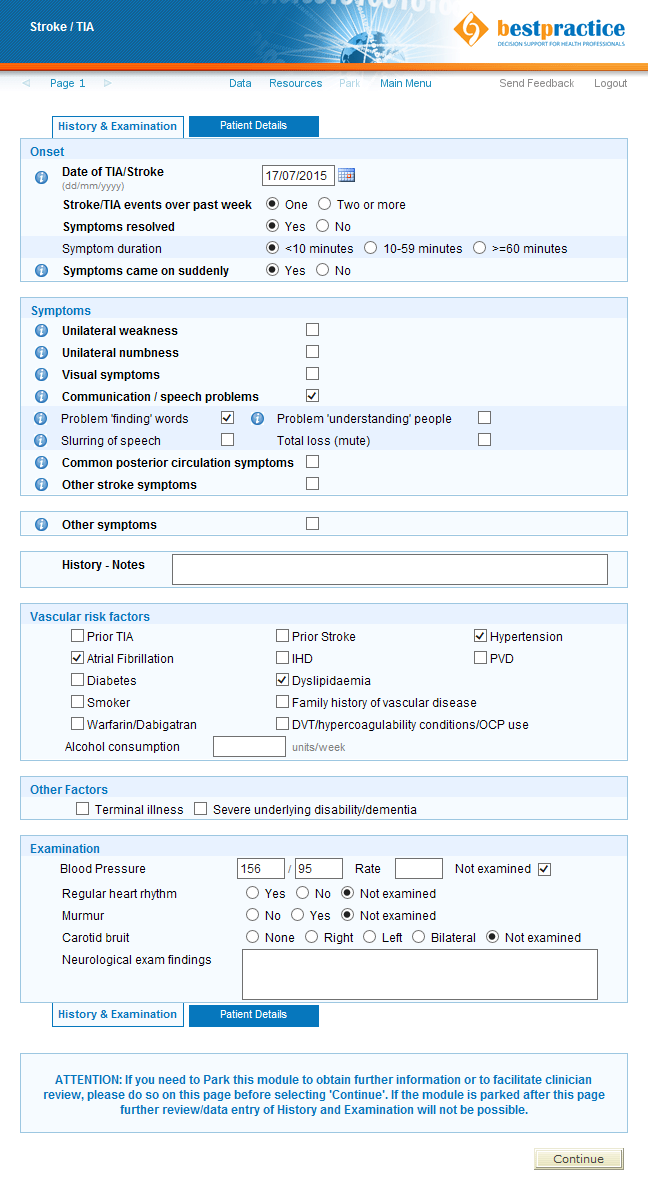
Above: The new TIA/Stroke electronic decision support data entry form showing a sample case.
The product bestpractice Decision Support has been developed by BPAC Inc, which is separate from bpacnz. bpacnz bears no
responsibility for bestpractice Decision Support or any use that is made of it.
 For further information about bestpractice Decision Support see:
www.bestpractice.net.nz
For further information about bestpractice Decision Support see:
www.bestpractice.net.nz