In this article 
View / Download
pdf version of this article
Key reviewer: Dr Amanda Oakley, Specialist Dermatologist and Clinical Associate Professor, Tristram
Clinic, Hamilton
| Key concepts |
- Use topical corticosteroids at the lowest potency possible to control the condition being treated
- Underuse of topical corticosteroids is much more common than overuse - use a “fingertip unit” for dosing
- The risk of adverse effects increases with potency, amount and length of time used
|
Topical corticosteroids are used for many skin conditions (Table 1). They suppress the inflammatory
reaction and relieve symptoms however they are not curative and when they are discontinued symptoms can recur.1
Topical corticosteroids should not be used for rosacea or acne vulgaris. They may worsen ulcerated or secondarily infected
lesions.1
Which potency do I choose?
In general use topical corticosteroids at the lowest potency possible to control the condition.
Low potency corticosteroids are typically used when treating large areas or for longer term application. They are also
more suitable for use on children or areas of thinner skin such as the face, groin or axilla.2
More potent corticosteroids are suitable for severe conditions and for use on areas of the body that have thicker skin
such as the palms of the hands and soles of the feet. They should generally not be used under occlusion or on areas of
thinner skin.2
Occlusion increases the absorption of topical corticosteroids by increasing the hydration of the skin and therefore
enhancing penetration. This needs to be considered when selecting corticosteroid potency. Occlusive materials include
polyethylene gloves, plastic film (e.g. Gladwrap) or occlusive dressings.3 Irritation, folliculitis and infection
are more likely to occur under occlusion.2 Corticosteroid related adverse effects are also more likely, especially
if occlusion is prolonged, because of increased absorption.
Which formulation do I choose?
Choice of formulation depends on a number of factors, including the type of skin lesion to be treated and its location.
Patient preference is important to consider because it can affect compliance.
Ointments are greasy and remain on the skin after they are applied. They are particularly suitable for use on dry, thick
or lichenified skin. The potency of a corticosteroid can be affected by its formulation e.g. for any given strength of
corticosteroid, an ointment formulation will be more potent than a cream. This is because the occlusive nature of an ointment
enhances absorption of the corticosteroid.2
Creams are often preferred by patients especially for use on exposed areas such as the face because they vanish when
rubbed into the skin.1,4 They are suitable for moist or weeping lesions. Creams contain more preservatives
and excipients than ointments and so are more likely to cause hypersensitivity or irritation.4
Lotions have a thin consistency, making them easier to apply to hairy areas such as the scalp.1 They contain
alcohol and have a drying effect on exudative lesions, but may sting on application.
| Table 1: Conditions that may respond to topical corticosteroids2 |
| Moderate - high potency corticosteroids |
Low - moderate potency corticosteroids |
Alopecia areata
Atopic dermatitis
Contact dermatitis (severe)
Discoid lupus
Hyperkeratotic eczema
Lichen planus
Lichen sclerosus
Lichen simplex chronicus
Exudative nummular (discoid) eczema
Psoriasis
Severe hand eczema
Stasis dermatitis |
Perianal inflammation (severe)
Asteatotic eczema
Atopic dermatitis
Dry nummular (discoid) eczema
Intertrigo (short-term)
Scabies (after scabicide)
Seborrhoeic dermatitis |
| Low potency corticosteroids |
Dermatitis (face, eyelids, napkin area)
Intertrigo
Perianal inflammation |
How much do I prescribe?
Underuse of topical corticosteroids is much more common than overuse. An acute or severe condition that is likely to
respond to topical corticosteroids should be treated generously, aiming to get control promptly.
Figure 1: Fingertip unit.
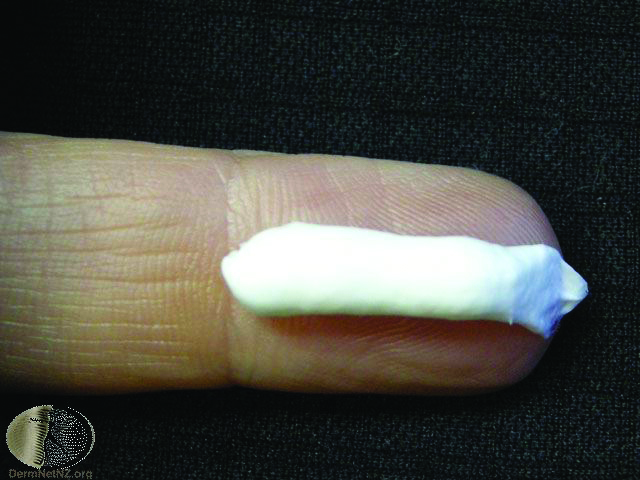 |
Regularly review patients with chronic skin conditions e.g. atopic dermatitis, to monitor use of topical corticosteroids
– they may be using excessive potency or frequency or quantities where a milder preparation or an emollient would be more
suitable. Conversely, the patient may be underusing topical corticosteroids because of perceived lack of efficacy, or
fear of adverse effects – generous intermittent applications of potent products should be encouraged e.g., “weekend
pulse therapy”.
Dose using fingertip units
A fingertip unit is a guide to how much corticosteroid to apply to a particular area and describes the amount of product
squeezed onto the top third of the finger (see Figure 1).5
Table 2: Number of fingertip units per body part5
| Body part |
Fingertip units |
Approximate quantity to prescribe* |
One hand
|
1 |
15 g
|
| One arm |
3 |
30 g
|
| One foot |
2 |
15 g
|
| One leg |
6 |
50 g |
| Face and neck |
2.5 |
30 g
|
| Trunk, front and back |
14 |
100 g
|
| Entire body |
~40 |
300 g |
| * for single daily application for an adult for two weeks |
One fingertip unit is equivalent to approximately 0.5 g for a male and 0.4 g for a female. Infants and children should
use one quarter to one third of the adult amount.
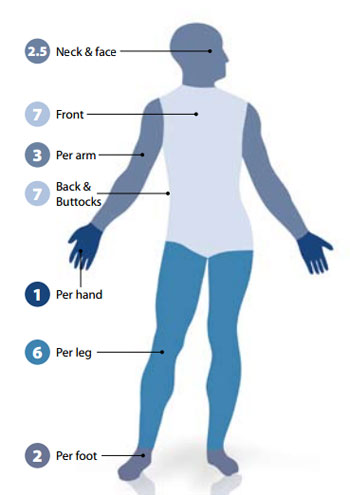
The number of fingertip units needed varies with the area of skin requiring treatment (Table 2 and Figure 2).
The amount of cream required daily can be used to calculate the correct amount needed on a prescription.
For example: If an adult female applies cream to both arms and hands once daily, she will need 3.2 g per day (i.e. eight
fingertip units × 0.4 g = 3.2 g per day) and 22.4 g per week. A 50 g tube should last approximately two weeks, but if
she applies it twice daily it will be finished in approximately one week.
How often should topical corticosteroids be applied?
Application of topical corticosteroids is usually recommended once or twice daily depending on the condititon being
treated.6 For the treatment of atopic eczema, applying topical corticosteroids more often than once daily has
not been shown to produce significantly better results and may adversely affect patient compliance.7
 Best practice tip: Prescribe moderate, potent or very potent topical corticosteroids
for once daily use only.
Best practice tip: Prescribe moderate, potent or very potent topical corticosteroids
for once daily use only.
How long can topical corticosteroids be used?
Long term use of topical corticosteroids can induce tachyphylaxis (tolerance to the vasoconstrictive action of topical
corticosteroids). Adverse effects are uncommon when using mild to potent corticosteroids for less than three months, except
when used on the face and neck, in intertriginous areas (skin folds), or under occlusion. However, very potent corticosteroids
should not be used continuously for longer than three weeks.2 If longer use of very potent corticosteroids
is required, they should be gradually tapered to avoid rebound symptoms and then stopped for a period of at least one
week after which treatment can be resumed.2
What adverse effects are likely to occur?
The risk of adverse effects increases with potency, the amount of topical corticosteroids used and occlusion. While
systemic adverse effects are rare, local adverse effects are more common and include skin atrophy, telangiectasia (especially
on the cheeks), acne and corticosteroid or preservative-induced contact dermatitis.9
Systemic adverse effects, including adrenal suppression, growth retardation, Cushing's syndrome and hypertension may
occur with the use of topical corticosteroids but are very rare. Cataracts and glaucoma have been reported in some cases
when topical corticosteroids, including hydrocortisone, have been used for long periods in the periorbital area.3
Adverse effects are more likely when topical corticosteroids are used:
- In infants and children
- For prolonged periods
- At high-potency
- Over large areas and under occlusion
References
- British National Formulary 56 ed. London: British Medical Association and the Royal Pharmaceutical Society of Great
Britain, 2008.
- Ference JD, Last AR. Choosing topical corticosteroids. Am Fam Phys 2009;79(2):135.
- Lee M, Marks R. The role of corticosteroids in dermatology. Australian Prescriber 1998. Available from:
http://www.australianprescriber.com/ (Accessed
June 2009).
- National Prescribing Service. Using topical corticosteroids in general practice. MeRec Bulletin 1999;10(6):21-24.
- DermNet NZ. Fingertip unit 2006. Available from: http://dermnetnz.org (Accessed
June 2009).
- National Institute for Clinical Excellence (NICE). Atopic eczema in children: management of atopic eczema in children
from birth up to the age of 12 years. 2007. Available from www.nice.org.uk (Accessed
June 2009).
- Williams HC. Established corticosteroid creams should be applied only once daily in patients with atopic eczema.
BMJ 2007;334:1272.
- Dermatology UK. Best practice in emollient therapy: a statement for healthcare professionals. Dermatology UK Ltd
2007. Available from: www.dermatology-uk.com (Accessed June
2009).
- Clinical Knowledge Summaries. Eczema - atopic 2008. Available from:
http://cks.library.nhs.uk/eczema_atopic/ (Accessed
June 2009).
- DermNet NZ. Topical corticosteroids 2007. Available from: http://dermnetnz.org/ (Accessed
June 2009).