In this article 
View / Download
pdf version of this article
Key reviewer: Dr Amanda Oakley, Specialist Dermatologist and Clinical Associate Professor, Tristram
Clinic, Hamilton
| Key concepts |
- Psoriasis is an emotionally and physically debilitating disease which can significantly affect quality of life
- Psoriasis is aggravated by factors including smoking, high alcohol intake, high glycaemic diet, certain medications
(particularly lithium) and emotional stress
- Management includes support with the psychosocial aspects of the disease and advice on lifestyle interventions
|
- Topical treatments are the first choice for mild psoriasis, and are also used adjunctively for resistant lesions
in patients with more extensive disease
- Calcipotriol and intermittent potent topical corticosteroids are prescribed for the majority of patients
- Systemic treatments are used for severe disease and are usually initiated by specialists
|
Psoriasis is an immune-mediated chronic scaly skin disorder in which there is upregulation of protein expression resulting
in excessive keratinocytic proliferation, abnormal keratinocyte differentiation and inflammation. The pathogenesis involves
Tumour Necrosis Factor (TNF)-α, dendritic cells and T cells. Normally keratinocytes require 28 – 44 days to migrate from
the basal cell layer of the epidermis to the stratum corneum, but in people with psoriasis this migration takes only four
days. Excessive cornification hardens the surface of the thickened plaques, which are red because of prominent vascularity.
Psoriasis is one of the most prevalent autoimmune diseases affecting both men and women equally. Approximately 2–3%
of the New Zealand population are affected. Psoriasis most often appears in the late teens or in the 50s, but can develop
at any age. There is a genetic predisposition and approximately one third of people with psoriasis report having an affected
relative.1,2
It is an emotionally and physically debilitating disease which can have a significant impact on quality of life and
can lead to depressive illness. Up to 25% of patients with psoriasis may also have seronegative arthritis.2 It
is associated with diabetes mellitus and people with moderate and severe psoriasis have a three-fold increased risk of
cardiovascular disease.3 Aggravating factors include smoking, high alcohol intake, high glycaemic diet, certain
medications (e.g. lithium, beta-blockers) and emotional stress.4
Assessing Severity
Severity can be defined by how much of the body surface area is affected:
5
- Mild psoriasis: < 5% of the body surface area
- Moderate psoriasis: 5–10% of the body surface area
- Severe psoriasis: >10% of the body surface area
Quality of life is also taken into consideration when assessing severity.
 Best practice tip: To estimate the percentage of body surface area
affected by psoriasis, consider that the palm of your hand (excluding fingers) is approximately equal to 1% of your body
surface area.
Best practice tip: To estimate the percentage of body surface area
affected by psoriasis, consider that the palm of your hand (excluding fingers) is approximately equal to 1% of your body
surface area.
Diagnosis and monitoring
Psoriasis is diagnosed clinically, occasionally with the support of histology. There are no specific blood tests to
diagnose or monitor psoriasis. Cardiovascular risk should be monitored due to the association between cardiovascular disease
and psoriasis.3
There are several different types of psoriasis
There are several different types of psoriasis (Box 1). It may be widespread or localised to one part of the body, such
as the scalp or fingernails. Psoriasis affecting the face, hands and feet may be particularly debilitating.
One way to assess severity depends on how much of the body surface is affected (see box “Assessing Severity”).
Clinical trials may use the more complex Psoriasis Area and Severity Index (PASI) score to assess effectiveness of treatment.4
Box 1: The main clinical types of psoriasis4
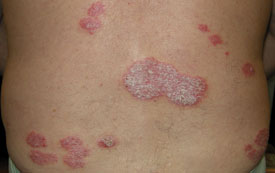
| Plaque psoriasis (psoriasis
vulgaris) – most prevalent form (~ 80%), thin to thick red plaques covered with a silvery scale, typically found on
the elbows, knees, scalp and lower back but may occur anywhere. Most (~ 80%) people affected with plaque psoriasis
have mild to moderate disease. |
 |
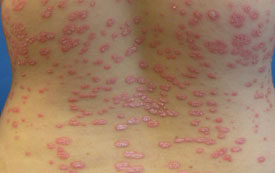
| Guttate psoriasis – 5 to 10 mm red plaques on the
trunk and limbs, often appearing suddenly after a Streptococcal or viral upper respiratory tract infection. |
 |
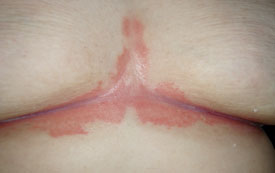
| Flexural psoriasis – bright red smooth shiny skin
lesions found in skin folds: axillae, groin, under breasts and around genitals and buttocks. |
 |
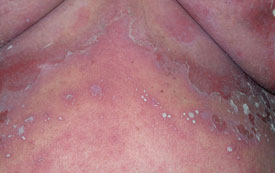
| Generalised pustular psoriasis – a severe acute
illness characterised by fever associated with crops of sterile pustules arising in or around painful red skin. It
can be triggered by systemic or potent topical steroids and other medications, over-exposure to UV light, infections
and stress. |
 |
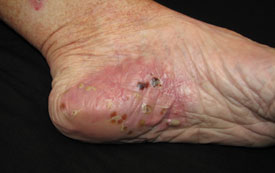
| Palmoplantar pustulosis – sterile pustules arising
on palms and soles strongly associated with smoking (95%). Chronic plaque psoriasis is associated in 25% of cases. |
 |
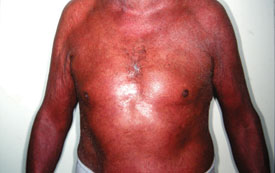
| Erythrodermic psoriasis – a particularly inflammatory
form of psoriasis that affects most of or the entire body surface and can lead to hypothermia, hypoalbuminaemia and
cardiac failure. Severe cases require hospitalisation. Known triggers include the abrupt withdrawal of a systemic psoriasis
treatment, allergic reactions, over-exposure to UV light, infection and some medications (e.g lithium, antimalarials). |
 |
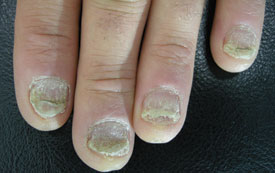
| Nail psoriasis – pitting, onycholysis, subungual
hyperkeratosis and other forms of nail dystrophy affect about 50% of patients with other forms of psoriasis. |
 |
| Pictures supplied by DermNet NZ |
Management
Educating the patient about the chronic nature of psoriasis and possible co-morbidities is important. Reassure them
that it is not contagious and that treatment can help. The patient may require support to cope with the psychosocial aspects
of the disease. Some patients may choose not to treat the skin disease itself as treatments can be burdensome and associated
with adverse effects.
Provide general advice regarding the benefits of not smoking, maintaining optimal weight and avoiding excessive alcohol.
Although sun exposure is often helpful, fair skinned people should be cautioned regarding the risk of sunburn and long
term overexposure, leading to aging of the skin and skin cancer.
Treatment has to be individualised. It will vary depending on the characteristics of the psoriasis being treated: its
body location, thickness of lesions, degree of erythema and scale, as well as patient preference or commitment to therapy.
Topical treatments are the first choice for mild psoriasis, and are also used adjunctively for resistant lesions in
patients with more extensive disease (who are being treated with phototherapy and/or systemic medications).
Treatments most commonly initiated in general practice include:
- Topical skin therapies:
- Corticosteroids
- Calcipotriol
- Dithranol
- Coal tar/pine tar (see below for a list of products)
- Scalp treatment
- Nail treatment
Topical skin therapies
Regular use of a thick emollient such as fatty cream is helpful to prevent cracking and irritation. Emollients may be
supplemented by keratolytic or “descaling” agents, such as 10% urea cream or 2% salicylic acid in white soft
paraffin.
Coal tar or pine tar emollient solutions in bathwater may be soothing, reduce itch and allow gentle removal of scale.
Corticosteroids
Topical corticosteroids are used by the majority of people with psoriasis, particularly those with limited disease.
Corticosteroids have anti-inflammatory, immunosuppressive and antiproliferative properties.
Lower potency corticosteroids should generally be used for limited periods of time on the face and other areas of thin
skin and in infants. Pimecrolimus is an alternative anti-inflammatory cream for psoriasis affecting the face or genitals,
but is not effective on other sites where plaques are thick.
In other areas and in adults moderate or high-potency corticosteroids are generally recommended as initial therapy.
Thick chronic plaques and plaques on hands and feet may require treatment with the highest potency agents (for a maximum
of three weeks). Ointments are the best choice for dry, scaly plaques.
One of the drawbacks of corticosteroid therapy is associated tachyphylaxis, leading to decreased efficacy with continued
use, and sometimes resulting in an acute flare-up when therapy is stopped. Once the lesions have improved, these effects
can be minimised by switching patients to less potent formulations, or advising them to apply the medication less frequently,
i.e. for two to three consecutive days each week. Another strategy is the use of corticosteroid-free times.
Calcipotriol ointment/cream/scalp solution
Calcipotriol (Daivonex, fully subsidised) is a vitamin D analogue that acts mainly by reducing the proliferation of
keratinocytes. Treated areas become less scaly but may remain red.
It is not recommended for severe extensive psoriasis unless calcium status is carefully monitored, because of the risk
of hypercalcaemia secondary to excessive absorption of calcipotriol.6
Calcipotriol cream or ointment (50 mcg/g) can be applied topically to chronic plaques twice daily. It may be reduced
to once daily when the condition improves, however it is most effective if applied consistently twice daily.
Calcipotriol is not as well absorbed from the cream formulation as the ointment, so the cream is only used if there
is a strong patient preference.
Safety of calcipotriol.6 The most common adverse effect is localised skin irritation, which may lessen with
continued use.
Calcipotriol is not usually recommended for use on the face because it may cause itching and erythema of the facial
skin. However some patients are able to use the cream formulation successfully on the face. Irritation may be reduced
with hydrocortisone cream. When patients are applying calcipotriol to other parts of their body, they should be advised
to wash their hands after application, to avoid inadvertent transfer to the face.
Hypercalcaemia has been reported rarely at the recommended dose, however serum calcium and renal function should be
monitored at three monthly intervals, if patients are applying larger quantities. To avoid the risk of hypercalcaemia,
calcipotriol should not be used concurrently with calcium or vitamin D supplements.
Calcipotriol total dose should not exceed 5 mg/week, for example:
- 100 g of ointment or cream
- 60 mL of scalp solution plus one 30 g tube of cream or ointment
- 30 mL of scalp solution plus two 30 g tubes of cream or ointment
Direct sunlight and UV radiation may inactivate calcipotriol, so it is best applied after exposure.
Note that calcipotriol is poisonous to dogs.
Calcipotriol use in children. Calcipotriol (50 mcg/g) can be used in children aged six years and over
but the datasheet indicates it should not be used for more than eight weeks.6
For children aged 6–12 years the maximum weekly dose should not exceed 50 g, while for children over 12 years the maximum
weekly dose is 75 g.
Combined use of calcipotriol and other psoriasis treatments. When using multiple topical treatments,
instruct patients to apply them at separate times. For example a topical corticosteroid may be used in the morning and
calcipotriol used in the evening or calcipotriol may be used twice daily on weekdays, and the topical corticosteroid twice
daily at weekends.4,5
Calcipotriol should not be used at the same time as topical salicylic acid because it is inactivated by it.4
Dithranol7
Dithranol (Micanol cream, fully subsidised) belongs to the family of hydroxyanthrones which have been used in the treatment
of psoriasis for more than a century. In the archaic Ingram regimen, a thick paste is applied to large plaques twice daily,
under carefully applied dressings. It is then removed in a tar bath and the patient exposed to UV radiation. This regimen
is too difficult for home use as dithranol is very irritating to normal skin and causes permanent stains on clothing and
bathtubs.
A short-contact regimen may be suitable for well motivated patients with small numbers of large plaques of psoriasis.4 Dithranol
1% cream can be applied once daily to the plaques, rubbed in gently until it no longer smears, and rinsed off (water only)
after 10 minutes. The application time can be increased gradually over seven days to a maximum of 30 minutes.
It should not be applied to areas of thin skin (such as face, genitalia, intertriginous areas) and should be avoided
in pregnancy, lactation and in children. Patients should be reminded that it can cause staining of skin, hair, fingernails
(gloves are recommended when applying it), clothing and bed linen. If redness or burning occurs the treatment should be
reduced or stopped.
Coal tar/pine tar
It is not well understood how coal or pine tar works for psoriasis, but it appears to have an anti-pruritic nature and
is keratoplastic – i.e. it normalises keratin growth in the skin to reduce scale build up.4
Coal and pine tar are used mainly as a bath additive or scalp application. Coal or pine tar preparations or Egopsoryl
TA gel (unsubsidised) can be directly applied to plaques. Coal or pine tar is often combined with salicylic acid 2 – 4%
as a keratolytic. See below for a list of products.
 Best practice tip: LPC (coal tar solution) and/or salicylic acid
may be prescribed in an emulsifying ointment base for chronic plaques on the trunk or limbs or in aqueous cream for application
to the scalp. For example, a prescription may be written as: “LPC 10%, salicylic acid 2% in aqueous cream ad 100%.
200 g”.
Best practice tip: LPC (coal tar solution) and/or salicylic acid
may be prescribed in an emulsifying ointment base for chronic plaques on the trunk or limbs or in aqueous cream for application
to the scalp. For example, a prescription may be written as: “LPC 10%, salicylic acid 2% in aqueous cream ad 100%.
200 g”.
Scalp treatments
Ketoconazole (2% shampoo) may help some patients with diffuse mild scalp psoriasis, although it is more effective in
seborrhoeic dermatitis.4 It is used twice weekly and is best left on the scalp for several minutes before rinsing
off.
Coal tar/pine tar shampoos (e.g. Neutrogena T/Gel, Polytar Plus, Fongitar, Ionil-T, Sebitar) are unsubsidised but generally
more effective than ketoconazole shampoos. They are used one to two times per week (or as necessary) and are best left
on the scalp for several minutes before rinsing off.
Coco-scalp (fully subsidised) is an ointment made from coal tar, sulphur, salicylic acid and coconut oil that can be
applied to scaly plaques and left for a minimum of one hour before washing off. It can safely be occluded (e.g. wrapping
the hair in plastic cling film) for several hours to achieve better de-scaling results.
Alternatively, in patients with coal tar intolerance or aversion, try salicylic acid 2–4% in aqueous cream, washed out
after several hours.
Dithranol 0.1% can be applied to the scalp, after the hair has been washed to remove any grease and
while the hair is still damp, and rinsed off (water only) after 30 minutes. It is unsuitable for blonde or grey hair as
it may stain.
Corticosteroid scalp applications include (in increasing potency):
- Hydrocortisone-17-butyrate 0.1% (Locoid Scalp Lotion or Crelo)
- Betamethasone valerate 0.1% (Beta Scalp application)
- Mometasone furoate 0.1% (Elocon Lotion)
- Clobetasol propionate 0.05% (Dermol Scalp application)
Topical corticosteroids are applied to the scalp once or twice daily for short courses up to one month in duration,
and then two to three days each week for maintenance if required. Overuse may cause psoriasis to worsen. Topical corticosteroids
are particularly useful to reduce pruritus although alcohol-based lotions may sting on application and they are ineffective
through thick scale.
Calcipotriol scalp solution (50 mcg/mL) can be applied topically to the scalp twice daily, reducing
the frequency when improvement occurs. Dose of the solution should not exceed 60 mL per week. If cosmetically acceptable
to the patient, calcipotriol in a cream base may be more effective than the solution.
Nail treatments
Treatment of nail psoriasis is often ineffective.4 Topical scalp preparations (corticosteroids and calcipotriol)
can be dripped or rubbed under affected nails and rubbed into the proximal nail fold. The patient should be advised that
it may take months or longer for results as nails grow slowly (e.g. 1 mm per month).
Coal/pine tar preparations used for psoriasis
Coal tar can irritate the skin so patients need to experiment with different products. A higher concentration of coal
tar is more effective but has a greater risk of irritation.
| Preparations |
Quantities and other ingredients |
| For application to scalp |
Coco-scalp ointment  |
Coal tar solution 12%, sulfur 4%, salicylic acid 2%, coconut oil
|
Fongitar shampoo 
|
Pyrithione zinc 1%, Polytar 1% (tar 0.3%, coal tar solution 0.1%, cade oil 0.3%, arachis oil extract
of crude coal tar 0.3%) |
Ionil-T shampoo  |
Salicylic acid 2%, coal tar solution 5% |
Neutrogena T/Gel shampoo  |
Coal tar 0.5% (as solubilised coal tar extract 2%) |
Polytar Plus shampoo  |
Coal tar 4% |
Sebitar shampoo  |
Pine tar 1%, coal tar solution 1%, salicylic acid 2% |
| For bathing |
Polytar Emollient liquid  |
Polytar 25% (tar 7.5%, coal tar 2.5%, cade oil 7.5%, arachis oil extract of crude coal tar 7.5%),
liquid paraffin in a water dispersible base |
Polytar Liquid  |
Polytar 1% (tar 0.3%, coal tar solution 0.1%, cade oil 0.3%, arachis oil extract of coal tar 0.3%) |
For application directly to plaques
|
Egopsoryl TA gel  |
Coal tar solution 5%, sulfur 0.5%, phenol 0.5%, menthol 0.75%, allantoin 2.5% |
Key: :  fully subsidised; : fully subsidised; :
 partially
subsidised; : partially
subsidised; :  not subsidised not subsidised |
Specialist referral
Referral for phototherapy or systemic therapy should be considered for those with:
- More than 10% to 20% body surface involvement
- Generalised pustular psoriasis (mild, localised or palmoplantar pustulosis may not require referral)
- Erythrodermic psoriasis
- Psoriatic arthritis
- Localised recalcitrant psoriasis
- Psoriasis that significantly interferes with function e.g. on the palms or on the soles of feet
Specialist initiated treatments include phototherapy (narrowband UVB), methotrexate, acitretin,* ciclosporin
and biological response mediators (e.g infliximab, adalumimab). Photochemotherapy (PUVA) has been discontinued in most
centres except for use in localised hand and foot treatment.
Systemic therapies are not always effective and they may have potential serious adverse effects and risks.
Phototherapy
Narrowband UVB phototherapy is available in larger hospitals and some private dermatological practices. The patient
stands in a cabinet containing 24 to 56 fluorescent bulbs, primarily emitting a wavelength of 311–312 nm, and is exposed
to increasing doses two or three times weekly for 20 to 40 treatments. Thin plaque psoriasis responds best with about
85% of patients achieving 90% clearance. Prolonged remissions are common. Risks of this therapy include burns, presumed
increase in skin cancer and premature aging of the skin.5
Methotrexate
Methotrexate is a folate antagonist and T-cell suppressive. It is effective for at least 60% of patients with psoriasis,
taken as a weekly dose of 10 to 30 mg. Supplementary folic acid (5 mg once weekly) may reduce the risk of adverse effects
such as gastrointestinal disturbance and mouth ulceration. Methotrexate is absolutely contraindicated in pregnancy and
lactation. It also affects sperm and men should not father children while taking it. Significant liver disease, especially
when resulting from alcohol misuse, precludes treatment. Other folate antagonists such as trimethoprim and sulfonamides
must not be prescribed with methotrexate, because of an increased risk of marrow suppression.
Monitoring blood count, liver function and serum creatinine every one to three months is essential. Long term liver
fibrosis and cirrhosis is a risk and additional specialist monitoring may be required.
Acitretin
Acitretin is a synthetic aromatic analogue of retinoic acid. It acts by normalising epidermal cell proliferation, differentiation
and cornification. It is particularly useful for erythrodermic and pustular forms of psoriasis. The thickness and scaling
of chronic plaque psoriasis usually improves on treatment. Like isotretinoin, it has recently become fully funded when
special authority criteria are fulfilled. However there are significant adverse effects and risks from treatment.
The initial dose is 10–30 mg daily and the maintenance dose depends on clinical efficacy and tolerability.
Safety of acitretin.8 Acitretin is highly teratogenic and must not be used by women who
are pregnant, or of child bearing potential, unless strict contraception is used for four weeks before, during
and for three years after treatment. Blood donation is prohibited during, and for one year after completion of
therapy.
Alcohol must be avoided during treatment and for two months after treatment with acitretin, particularly by women of
child bearing potential. This is because it can lead to the formation of etretinate, a retinoid that is stored in fat
cells, and takes several years for the body to clear.
Acitretin is contraindicated in patients who are breastfeeding, or those with severely impaired renal or hepatic function,
or chronically abnormal elevated blood lipid values.
Tetracyclines, methotrexate and vitamin A or other retinoids must be avoided.
Hepatic function and serum lipids should be regularly monitored throughout treatment. Acitretin may result in a reversible
hyperlipidaemia requiring active management. People with diabetes may experience a change in their glucose tolerance (both
improvement or worsening can occur) and so blood glucose levels may require more intensive monitoring in the early stages of treatment.
The most common adverse effects observed are dryness of the lips, epistaxis, peeling palms and soles, dry skin, asteatotic
dermatitis and diffuse hair loss (which may be severe). These are symptoms of hypervitaminosis A. Many patients are unable
to tolerate acitretin because of fatigue, myalgia, arthralgia or ophthalmic effects (e.g. blurred vision, impaired night
vision).
Ciclosporin
Ciclosporin is rapidly effective for psoriasis in doses ranging from 2.5 to 5 mg/kg/day, taken for three to six month
courses. However, as psoriasis tends to relapse quickly on discontinuing the drug, many people take it for prolonged periods
risking hypertension, renal impairment, increased risk of skin cancer and other adverse effects.
Monitor blood pressure and renal function regularly, along with other routine tests (see BPJ
17, October 2008 “Monitoring DMARDs”).
Biological response mediators
Several proteins and monoclonal antibodies that target T cells and TNF-α have come on to the market in the last decade
and many new drugs are under investigation. Treatment is well tolerated and often very effective for psoriasis. Long-term
studies are ongoing to determine safety, as these agents may increase granulomatous infections, such as tuberculosis and
have been reported to exacerbate cardiac failure and demyelinating conditions (e.g. multiple sclerosis).9
Infliximab is a TNF-α inhibitor given as an intravenous infusion at weeks zero, two and six, then every eight weeks.
It is reserved for very severe psoriasis and can be administered in both hospital or outpatient settings.
Adalimumab is also a TNF-α inhibitor, self-administered as a subcutaneous injection every two weeks. Adalimumab is now
funded on Special Authority application (initially by a specialist) for small numbers of patients with severe psoriasis
in whom current treatments are ineffective or contraindicated.