Although there are many potential sources of exposure to mercury and its compounds, most people can be reassured that they are at low risk of mercury toxicity. The exception to this is the exposure of the developing foetal brain to organic mercury. Laboratory testing of mercury levels is generally not appropriate unless specific indications are present such as a history of mercury ingestion or occupational exposure.
In this article 
View
/ Download pdf version of this article
Occasionally patients may present to primary care expressing concern about mercury toxicity, or requesting testing
following their own research. Although there are many potential sources of exposure to mercury and its compounds, most
patients can be reassured that they are at low risk of mercury toxicity. The exception to this is the exposure of the
developing foetal brain to organic mercury.
Sources and risks of mercury exposure
Mercury exists in three different forms:1
- Elemental mercury (also known as quicksilver) – a silvery, shiny, volatile liquid, which emits a colourless, odourless
vapour at room temperature
- Inorganic mercury – compounds formed when elemental mercury combines with other elements such as sulphur, chlorine
or oxygen to create mercury salts
- Organic mercury – compounds that are formed when elemental mercury combines with carbon, such as methyl mercury
The adverse health effects of mercury exposure depend on its chemical form (elemental, inorganic or organic), the route
of exposure (inhalation, ingestion or skin absorption), and the level of exposure. Vapour from liquid elemental mercury
and methyl mercury are both more easily absorbed than inorganic mercury salts and are therefore more toxic.
Potential sources of exposure to mercury2
Elemental mercury:
- Inhalation and skin absorption when handling liquid mercury, e.g. broken thermometers, sphygmomanometers, fluorescent
light bulbs
- Amalgam dental fillings
- Environmental exposure, e.g. air contamination from burning coal and industrial waste
- Release from soil in geothermally active areas (low levels in New Zealand)
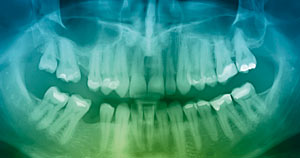
Amalgam dental fillings
Dental amalgam fillings contribute only a minor amount to the total mercury levels in the body, and do not cause a
significant increase in blood mercury level. There is no good evidence that amalgam fillings cause mercury toxicity.4
The American Dental Association (ADA) states that amalgam is a safe material with no sound scientific evidence supporting
a link between amalgam fillings and systemic diseases or chronic illness. The U.S Food and Drug administration group
(FDA) concludes that amalgam fillings do not significantly contribute to mercury-related toxicity. The FDA found that
in adults and children aged six years and over, who have fifteen or more amalgam surfaces, mercury exposure was far below
the lowest levels associated with harm.5 In addition the FDA does not recommend that amalgam fillings are
removed or replaced. Removing sound amalgam fillings results in unnecessary loss of healthy tooth structure, and results
in exposure to mercury vapour released during the removal process.
Although amalgam fillings are considered safe, research to develop new filling materials is ongoing.
Inorganic mercury salts:
- Non-prescription calcium supplements
- Some complementary medicines
- Topical agents such as bleaching creams to remove freckles
- Some fungicides
- Red colouring in some tattoos
Organic mercury salts:
Mercury in fish
Fish is by far the biggest source of exposure to organic mercury, in the form of methyl mercury. Organic mercury is
passed along the food chain from smaller fish to larger predator fish, e.g. swordfish, shark, tuna, which contain the
highest levels of accumulated mercury. Mercury levels can also be high in trout caught from geothermal lakes. Cooking
does not reduce mercury content in fish. All canned fish (including tuna, herring and mackerel) sold in New Zealand contain
acceptably low levels of mercury.2
The developing foetus, infants and young children are most susceptible to mercury-related neurotoxicity that may result
from consuming large amounts of fish. The New Zealand Food Safety Authority advises that pregnant women should choose
fish varieties with lower mercury concentrations.3 Fish that are likely to contain the lowest levels of mercury
include: farmed salmon, skipjack tuna, tarakihi, blue cod, hoki, john dory, monkfish, warehou, whitebait and flat fish
(e.g. flounder), as well as mussels and pacific oysters. Small, canned fish such as sardines and mixed fish (e.g. fish
portions and fish fingers) can also be eaten without restriction.
Symptoms of mercury toxicity
Low grade continuous exposure to mercury can lead to:6
- Inflammation of the mouth, soft gums, loose teeth, excessive salivation, metallic taste and foul breath
- Tremor (hatter’s shakes), particularly when the person is being observed or is in an unfamiliar environment
or job
- Mental and nervous symptoms including behavioural changes, stammering, anxiety, insomnia and loss of energy and drive
Laboratory testing of mercury
Appropriate indications for testing blood or urine mercury:4
- History of mercury ingestion (other than normal consumption of fish) or other exposure
- Occupational health monitoring
- Neurological symptoms suggesting occult mercury poisoning
Inappropriate reasons for requesting blood or urine mercury:4
- Non-specific symptoms such as memory loss, cognitive decline, depression or chronic fatigue syndrome
- The presence of amalgam fillings
- Autism spectrum disorder or Alzheimer’s disease (there is no convincing evidence that mercury is linked to either
of these conditions)
- Routine “screening” or an “annual check”
Blood mercury is the recommended test to diagnose mercury poisoning as most mercury is present in red
blood cells. Levels are raised by recent exposure, e.g. a large seafood meal may raise blood mercury, which then declines
over subsequent weeks. The half-life of organic mercury in blood after exposure is approximately seven to ten weeks and
three to 15 days after vapour exposure. After inorganic mercury exposure, the half-life is three to four weeks.2
Urine testing is used to assess chronic exposure to inorganic and elemental mercury. Organic mercury
exposure (i.e. through seafood ingestion) usually only has a minimal effect on urine mercury levels.
In a primary care setting, testing for mercury in other samples, e.g. hair, nails or cerebrospinal fluid, is difficult
and expensive, and is not recommended.
Acknowledgement
Thank you to Associate Professor James Davidson, Labplus, Auckland City Hospital for providing expert
guidance in developing this article.
References
- Health Canada Mercury Issues Task Group. Mercury and human health. March 2009. Available from:
www.hc-sc.gc.ca/hl-vs/iyh-vsv/environ/merc-eng.php (Accessed
Nov, 2010).
- Kyle C (editor). A handbook for the interpretation of laboratory tests. 4th Ed. Auckland: Diagnostic Medlab; 2008.
- New Zealand Food Safety Authority. Mercury in fish. Food Focus. November 2008. Available from: www.nzfsa.govt.nz/publications/food-focus/2008-11/page-13.htm (Accessed
Nov, 2010).
- Davidson J. Mercury testing: Fact Sheet. June 2010, Auckland City Hospital: Labplus; 2010.
- U.S. Food and Drug Administration (FDA). About dental amalgam fillings. Available from: www.fda.gov (Accessed
Nov, 2010).
- George PM, King R, Grant SJ, et al. Handbook of biological monitoring for health, 3rd ed, Christchurch, New Zealand:
Canterbury Health Laboratories; 2009. Available from: www.labnet.co.nz (Accessed
Nov, 2010).