Stroke is the third leading cause of death in New Zealand, after ischaemic heart disease and all cancers combined and is the most important cause of adult disability. Clearly a concerted effort is required across all population groups but there are specific issues for Māori, Pacific people and women.
In this article 
View / Download pdf
version of this article
Stroke is the third leading cause of death in New Zealand, after ischaemic heart disease and all cancers
combined, and is the most important cause of adult disability. Clearly a concerted effort is required across all population
groups but there are specific issues for Māori, Pacific people and women.
Trends in stroke rate show ethnic disparities
There has been a modest decline in the rates for both lifetime incidence of stroke and stroke attacks in Auckland over
the last two decades.1 This decline is consistent with the decline reported in Northern
European populations. However in Auckland the changes were not consistent across all ethnicities. Figure 1 clearly shows
the increasing rates of stroke attacks in Māori and Pacific peoples. What is more, the mean age at onset of stroke for
Māori is 60 years and Pacific people 65 years, compared to 75 years for New Zealanders of European ethnicity.2
Downward stroke trends linked to improved primary and secondary
prevention
Downward stroke trends reported among European populations have been attributed to improved primary and secondary prevention,
particularly improved blood pressure control, reduced cigarette smoking, lower cholesterol and greater use of blood pressure,
anti-platelet and cholesterol lowering medications.3
| Figure 1: Trends in ethnic-specific stroke attack rates by study period |
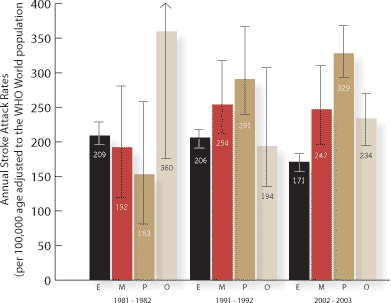 |
| Rates were age-standardised to the WHO world population and shown with 95% CI. |
Ethnic groups defined as:
E = NZ/European,
M = Maori,
P = Pacific peoples, and
O = Asian and other |
Favourable NZ trends for some risk factors counterbalanced
by obesity and smoking
The trends in some cardiovascular risk factors in New Zealand Europeans in Auckland were studied between 1982 and 2003.
4 Trends
in systolic blood pressure, raised blood pressure, serum cholesterol, HDL-cholesterol levels and use of antihypertensive
and cholesterol lowering drugs have generally been favourable. Unfortunately however these favourable trends were counterbalanced
by less favourable trends in body mass index, obesity and cigarette smoking.
Important risk factors for stroke
The important modifiable risk factors for stroke are:
- Hypertension
- Atrial fibrillation
- Diabetes
- Smoking
- Adverse lipid profile
Hypertension most important risk factor for stroke
Non-optimal control of blood pressure is the most important risk factor for stroke. There is a strong, direct and near-continuous
association between stroke incidence and level of blood pressure. Non-optimal control of blood pressure levels accounts
for almost two-thirds of the global burden of stroke.
Atrial fibrillation confers a five-fold increase in stroke risk
An estimated 15% of strokes are attributed to atrial fibrillation (AF) and when people with AF have a stroke they have
much worse outcomes. Stroke rates with AF are higher in women than in men, although men have slightly higher rates of
AF. Warfarin treatment is effective for both men and women but appears to be underused in women, although risk of major
bleeding appears to be no greater than in men.7
Warfarin significantly reduces the risk of stroke for people with AF but comes at a cost of increased bleeding risk.
Doctors appear to be poor at balancing the risks of stroke and bleeding6, even though
major bleeding can usually be managed by alteration of medication and a few days in hospital, whereas stroke is likely
to cause permanent disability or death.
Conclusions for primary care
The most cost-effective approaches for the primary prevention of stroke and other chronic diseases such as coronary
heart disease are population-based strategies to modify risk factors. However interventions during day-to-day consultations
also make a difference. Useful opportunistic strategies to add to any population-based strategies are:
- Opportunistic screening for risk factors during the consultation
- Starting this 10–15 years earlier for Māori, Pacific people and people from the Indian subcontinent
- Managing hypertension aggressively
- Checking for AF and managing it appropriately for both men and women
|