In this article 
View / Download
pdf version of this article
Motivational interviewing includes a range of techniques to help people make changes in their behaviour. It has been
shown to be effective in the primary care setting with smoking cessation, hazardous drinking, physical activity, nutrition
and chronic disease. This article provides an overview of motivational interviewing. Recommendations for further reading
can be found at the end of the article.
Motivational interviewing is based on the presumption that our behaviours are a product of our thoughts (what I know)
and our feelings (what I believe). For instance, knowing that something is bad for their health does not necessarily cause
a person to change their behaviour. For example, only 50% of smokers quit smoking after an myocardial infarction. To change
health behaviour we need to change feelings too.
Cycle of Change
Motivational interviewing helps people become motivated to change, moving through a cycle of change from belief that
a change is needed through to a belief in their ability to make change and stick to it.1
The components of the cycle of change are:
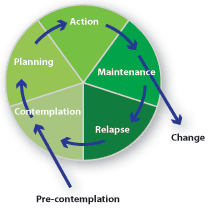
- Pre-contemplation: before thinking about change (Problem. What problem?)
- Contemplation: favourably disposed to change but have not made concrete plans (I'd like to, but...)
- Planning: strategies selected but not yet used (I have decided what to do.)
- Action: e.g. attempts made to stop smoking, lose weight, (I’m making changes.)
- Maintenance: sticking to it
Individuals can lapse at any stage and it is unusual to achieve permanent change in an ingrained behaviour at the first
attempt. Most people rotate through this cycle many times.
Motivational interviewing strategies
Motivational interviewing is about helping the patient make the decisions. It involves systematically directing the
patient towards motivation to change through empathic reflection, appropriate feedback and advice. The aim is to increase
the patients own internal conflict around the health related behaviour and their wish to change: “I want to” versus “I
don’t want to”.
Patients become motivated to change if they can see the benefits of change and that the costs of remaining the same
are high.
Empathic reflection
Motivational interviewing avoids confrontation and making judgements which tend to increase resistance to change. It
accepts that patients have their own reasons for choosing their behaviours and that there are costs and benefits which
can be highlighted to the patient. It starts with listening and expressing understanding, acceptance and interest.
Appropriate feedback and increasing internal conflict
Motivational interviewing lets the patient decide how much of a problem they have by selectively reinforcing the patients
own self motivational statements around problem recognition e.g. “I notice that you say everything is fine with
your drinking but that you say that it causes problems” and reinforcing the patients intention to change, “It
seems that you would like to try and change.” The aim is to highlight the patient’s own conflict between their
statements. It is often helpful to let the patient make the connection.
Areas of discrepancy may be helpfully summarised with a decision balance tool. This can be used to explore the patient’s
beliefs and motivation to change. Write down the patients likes and dislikes of the behaviour and the good and bad aspects
of changing:
Advice and encouragement
Work with the patient to plan small achievable goals by asking, “How can I help you?”
Summary
Throughout the process it is important to continually affirm the patient’s freedom of choice and self-direction.
Motivational interviewing is not about “making” people change but about motivating them to do so. We can provide
facts, offer advice and encouragement, a listening and empathic ear, and help explore their reasons for changing or not.
Motivational interviewing is a tool to use in the right circumstances to help people get closer to making permanent changes.
We do not fail if our patients do not make changes now.
Further reading
- The Royal Australian College of General Practitioners . Putting prevention into practice: Guidelines for the implementation
of prevention in the general practice setting (The Green Book) 2nd edition. July 2006. Available from:
www.racgp.org.au
- Britt E, Hudson SM, Blampied NM. Motivational interviewing in health settings: a review. Patient Educ Couns. 2004
May;53(2):147-55.
- The National Centre for Education and Training on Addiction (NCETA). Resource Kit for GP Trainer on Illicit Drug Use
3.4 Motivational Interviewing. Available from: www.primarymentalhealth.com.au
- Prochaska JO, DiClemente CC, Norcross JC. In search of how people change. Applications to addictive behaviors. Am
Psychol. 1992;47(9):1102-14.