The pathophysiology of nausea and vomiting is complex
The biological pathways that induce nausea and vomiting are complex (Figure 1).5 The nucleus tractus solitarius (NTS, or vomiting centre) is a cluster of neurons in the brainstem that mediates the vomiting reflex. These neurons receive input from various sources, including:5, 6
- The cerebral cortex, amygdala and limbic system – sensory input from higher centres relating to cognition and emotion, e.g. sights or smells that induce vomiting
- The chemoreceptor trigger zone (CTZ) – located in the medulla oblongata, near the fourth ventricle, sitting outside of the blood brain barrier. This region detects circulating abnormalities, e.g. medicines, bacteria or electrolyte imbalances in the blood and cerebrospinal fluid.
- The vestibular system – histamine-mediated signals resulting from inner ear dysfunction, e.g. motion sickness
- The gastrointestinal system – mechanoreceptors stimulated by gastric distension and chemoreceptors that detect bacteria, toxins, medicines in the gastrointestinal lumen
In response to information from the above pathways, the NTS sends signals via the vagal nerve to increase gastric contraction and relax the oesophageal sphincter leading to emesis.6, 7
The exact pathophysiology of nausea is less well understood but it likely involves the NTS receiving input from similar sites as listed above and then sending signals to the cerebral cortex to produce the sensation of nausea.5, 6
 Practice point: Clinicians should consider the likely pathophysiology of a patient’s nausea and vomiting when deciding on the most appropriate antiemetic to prescribe (Table 1).
Practice point: Clinicians should consider the likely pathophysiology of a patient’s nausea and vomiting when deciding on the most appropriate antiemetic to prescribe (Table 1).
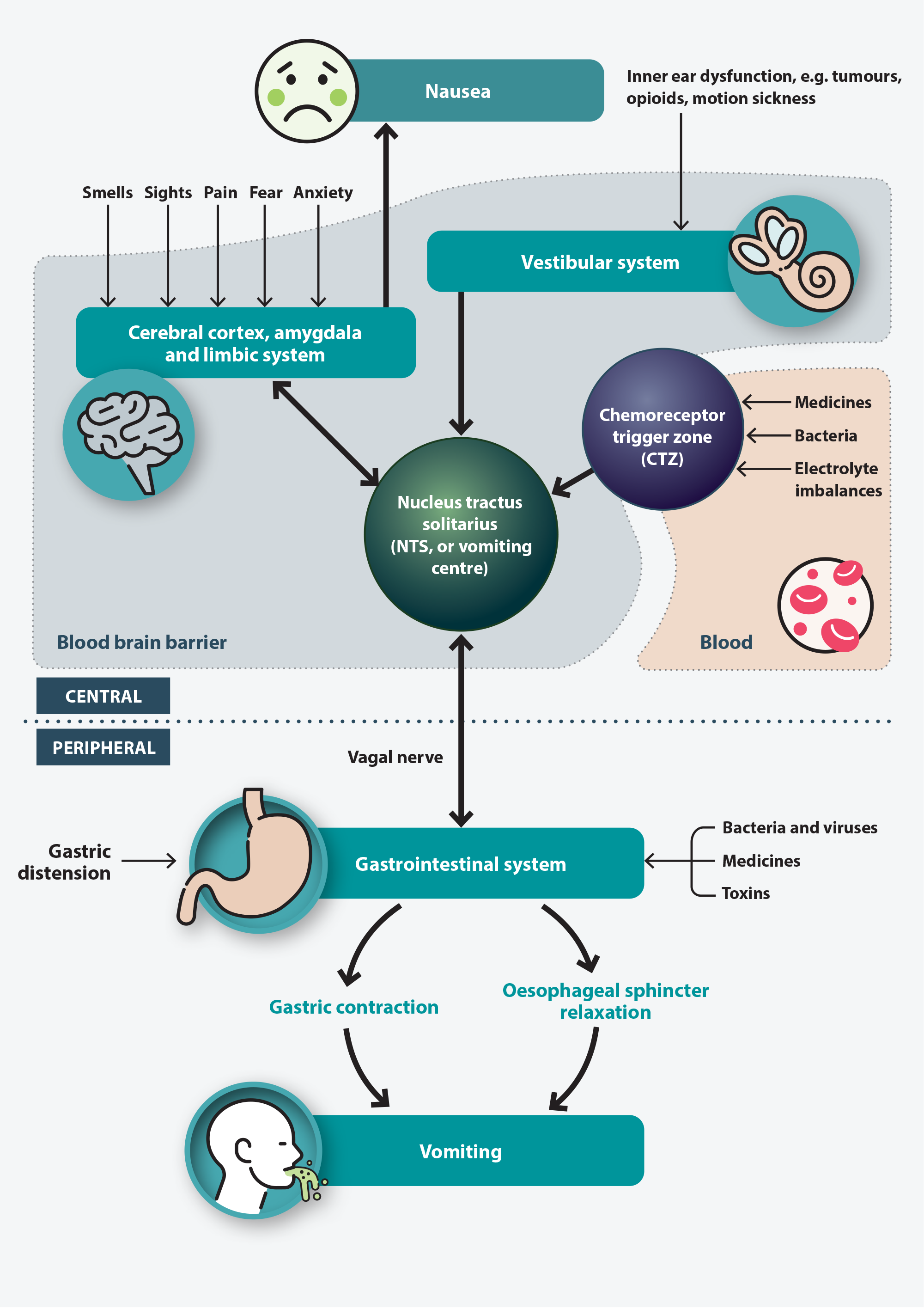
Figure 1. A simplified overview of the pathophysiology of nausea and vomiting.5-7
Assessing patients with nausea and vomiting
In patients with nausea or vomiting, consider the following factors during the baseline assessment (and ongoing reviews):1–3
- The onset, duration and severity of symptoms
- Potential triggers, e.g. smells from food preparation or those related to bodily functions
- Whether any of the patient’s medicines (for long-term conditions) are commonly associated with nausea or vomiting
- Whether the adverse effects of these medicines outweigh any potential benefit at this stage
- The presence of constipation or signs of faecal impaction, e.g. abdominal distension or mass, absence of bowel sounds
- Current hydration status and food and fluid intake
- The patient’s thoughts and emotions concerning their symptoms, e.g. fear, anxiety, anticipation
Discuss with the patient and their family/whānau that nausea and vomiting is not unexpected, why it occurs, and the treatment options that are available for them. Knowing what to expect can alleviate distress. Reassure family/whānau that food and fluid requirements reduce in the last days of life. Food and fluids should be offered but reducing portion sizes or modifying the consistency may be required (see: “Non-pharmacological management strategies for nausea and vomiting”).
Address modifiable causes early
Any modifiable causes of nausea and vomiting should be addressed first:8
Long-term medicines associated with nausea and vomiting include cardiac medicines (e.g. digoxin), NSAIDs and anticonvulsants.2, 3 Abrupt discontinuation of corticosteroids can result in adrenal insufficiency which may manifest as nausea.2 Non-essential medicines should be discontinued (if they have not been already),3 e.g. statins, oral hypoglycaemics. Possible exceptions include anticonvulsants or other medicines used to control symptoms, e.g. diuretics for heart failure, that could impact comfort or cause distress if withdrawn.9, 10
Constipation in the last days of life may be caused by medicines, dehydration, reduced food intake, limited movement or bowel obstruction.11 The benefit of pharmacological treatment may be limited at this time and is often not given, but if constipation is causing significant discomfort and thought to be contributing to nausea and vomiting, pharmacological treatment may be considered. Suppositories (e.g. bisacodyl, glycerol) or enemas (e.g. sodium citrate, phosphate) are preferred as oral medicines may no longer be appropriate.
N.B. If constipation is causing distress and treatment is not successful, a rectal examination may be appropriate to rule out faecal impaction or bowel obstruction resulting from a rectal tumour.10
Switching opioids in the last days of life may not be practical
Opioids are regularly prescribed for patients receiving end of life care.12 In some cases, the opioid may be able to be changed or the dose reduced if the usual adverse effects of opioids are intolerable, i.e. nausea, vomiting. However, in the setting of managing a patient in the community in the last days of life, often this is not practical, e.g. due to fixed doses established in syringe drivers, and higher doses needed to manage pain, therefore patients are usually managed by adding an antiemetic rather than withdrawing or changing the opioid. Patients who are vomiting and are currently taking oral opioids should be changed to subcutaneous delivery.13
Non-pharmacological management strategies for nausea and vomiting
Patient comfort is the main goal of management for nausea and vomiting. Non-pharmacological strategies to reduce nausea and vomiting include:1
- Positioning the patient upright when eating or drinking to reduce the likelihood of choking or aspiration
- Removing sights or smells that are known to trigger symptoms, e.g. certain foods, cooking aromas, deodorants/perfumes, air fresheners
- Adequate ventilation – open windows for fresh air, use of a fan
- Offering small quantities of food if the patient can still eat
- Some patients may want their favourite food while others may prefer bland foods
- Provide a variety of fluid options, e.g. water, juice, clear soup
- Using a straw may make fluid intake easier
- Offer ice blocks or ice chips if unable to tolerate oral fluids
- Occasionally, a nasogastric tube may be appropriate for patients with persistent vomiting.14 Discuss with the local hospice or palliative care team.
- Maintaining good oral hygiene – patients may benefit from regular mouth rinsing, brushing of teeth or cleaning of dentures
- Mouthwash can be made at home by mixing half a teaspoon of baking soda and half a teaspoon of table salt in 250 mL of water
- Relaxation and distraction techniques, e.g. listening to music, spending time with family/whānau
- Visualisation or guided imagery – allows patients to distance themselves from their symptoms; suggest they imagine themselves in a place associated with happy memories, e.g. favourite holiday spot
- Complementary or alternative remedies for nausea, e.g. ginger ale or peppermint tea
- Some patients may wish to include Rongoā Māori or other traditional remedies in their care, e.g. bark of the karamu plant (Coprosma robusta) for vomiting15
- The use of acupressure, either via family/whanau applying pressure to specific points or the use of wrist bands
Pharmacological management of nausea and vomiting
Pharmacological treatments are usually required in addition to non-pharmacological techniques to manage nausea and vomiting (Figure 2). Consider the most likely causes of a patient’s nausea or vomiting and the mechanisms of action of available antiemetics when deciding on the most appropriate treatment (Table 1 and see: “The pathophysiology of nausea and vomiting is complex”).10 Patients with multiple possible causes of nausea or vomiting may benefit from a combination of antiemetics;10 discuss with the local hospice or palliative care team.

Figure 2. Anticipatory prescribing for patients with nausea and vomiting. Adapted from South Island Palliative Care Workstream, 2020.8, 16
CSCI = continuous subcutaneous infusion
First-line treatment options for nausea and vomiting
If the patient is not currently taking an oral antiemetic, subcutaneous haloperidol (unapproved route) is an appropriate first-line pharmacological treatment option, unless contraindicated e.g. Parkinson’s disease, prolonged QT-interval.8, 16 Subcutaneous metoclopramide (unapproved route) or cyclizine (unapproved route) are alternative first-line antiemetics for patients who cannot take haloperidol.8 In practice, haloperidol is preferred in the last days of life as it has a lower risk of adverse effects in people who are frail compared to other first-line options and may have multiple indications, therefore reducing polypharmacy, e.g. it is also used to treat delirium.
Recommended doses:
- 0.5 mg haloperidol, subcutaneously every four hours, as needed (maximum dose 5 mg in 24 hours).8 N.B. The decision to switch to levomepromazine (see below) is usually considered if symptoms are not adequately controlled with 3 mg haloperidol, subcutaneously over 24 hours.
- 10 mg metoclopramide, subcutaneously every six to eight hours, as needed (usually recommended not to exceed 40 mg in 24 hours)8
- 75 – 150 mg cyclizine over 24 hours, via subcutaneous infusion (subcutaneous bolus doses are not recommended due the risk of injection site reactions17)16
Patients who are already taking an oral antiemetic should have their current regimen converted to subcutaneous doses which can be given either as bolus doses or over a 24-hour period using a continuous subcutaneous infusion (Table 1).8
Ideally, patients should be reassessed for treatment effectiveness and adverse effects within six hours.8 It is recommended to convert “as needed” doses to a 24-hour dose for continuous subcutaneous infusion in patients who experience an improvement in symptoms.8 Additional “breakthrough” subcutaneous doses of the antiemetic should also be prescribed.8
 Practice point: Ondansetron is not generally recommended to manage nausea and vomiting in patients receiving palliative care as it may exacerbate opioid-related constipation.2
Practice point: Ondansetron is not generally recommended to manage nausea and vomiting in patients receiving palliative care as it may exacerbate opioid-related constipation.2
Levomepromazine is a second-line treatment option for nausea and vomiting
Levomepromazine* is the most suitable option for patients with persistent nausea or vomiting (unapproved indication) despite taking the maximum tolerable doses of first-line antiemetics.8 It acts on multiple different receptors, making it suitable for patients with nausea and vomiting due a combination of causes.10
The previous antiemetic can be stopped and the patient switched to levomepromazine or it can be added to their regimen if there has been a partial effect from the previous medicine. The recommended initial dose is 3.125 – 6.25 mg of subcutaneous levomepromazine, every four to six hours, as needed (maximum dose 25 mg in 24 hours).8 If the patient requires more than two “as needed” doses in a 24-hour period, increase the dose.1 There is a risk of excessive sedation when higher doses of levomepromazine are used.18
*Previously known as methotrimeprazine
A combination of antiemetic medicines may be required for some patients
Nausea and vomiting often has multiple causes, making symptom management difficult.3 Patients who do not have a sufficient clinical response to a single antiemetic medicine may benefit from a combination of antiemetic medicines that act via different mechanisms of action (Figure 2).10 It is recommended to discuss patients with refractory nausea and vomiting with your local hospice or palliative care team.
 Practice point: Avoid prescribing anticholinergic medicines (e.g. cyclizine, hyoscine butylbromide) concomitantly with prokinetic medicines (e.g. metoclopramide) in patients with nausea and vomiting attributed to delayed gastric emptying as the anticholinergic effects may reduce the beneficial effects on gastric motility.3
Practice point: Avoid prescribing anticholinergic medicines (e.g. cyclizine, hyoscine butylbromide) concomitantly with prokinetic medicines (e.g. metoclopramide) in patients with nausea and vomiting attributed to delayed gastric emptying as the anticholinergic effects may reduce the beneficial effects on gastric motility.3
Prescribing benzodiazepines for nausea and vomiting
Benzodiazepines, e.g. midazolam, should be considered in patients whose nausea and vomiting may be related to fear or anxiety, e.g. administer beforehand if anticipation of a treatment or procedure is a likely cause of symptoms.3, 10
Table 1. Antiemetic medicines for managing nausea and vomiting in the last days of life.
| Medicine |
Dose |
Considerations |
Availability |
Haloperidol*
Dopaminergic (D2) receptor antagonist (at chemoreceptor trigger zone reducing the effects of circulating abnormalities)2, 10
In practice, the first-line antiemetic choice as lower adverse effect profile than alternatives, especially in frail or older people
Effective for opioid-induced nausea and vomiting, nausea as a result of end stage renal disease or hypercalcaemia10, 16 |
Patients not currently receiving an antiemetic:
0.5 mg, subcutaneously every four hours, as needed (usually do not exceed 3 mg/24 hours)
Patients already receiving oral haloperidol should be switched to:
0.5 – 1 mg, subcutaneously at night, or twice daily, as needed
OR
1 – 3 mg/24 hours, via CSCI. Patients whose symptoms are not adequately controlled with 3 mg haloperidol over 24 hours are usually switched to levomepromazine (occasionally a higher dose of haloperidol, e.g. up to 5 mg over a 24-hour period, may be beneficial). |
Contraindicated in Parkinson’s disease, prolonged QT-interval (gastrointestinal obstruction is a relative contraindication in the last days of life)8, 16
Avoid in patients with Lewy body dementia due to an increased risk of neuroleptic malignant syndrome19 |
5 mg/mL solution for injection (1 mL ampoules)
PSO and prescription |
Metoclopramide*
D2 and 5HT3 antagonist and 5HT4 agonist (at chemoreceptor trigger zone and peripherally promotes gastric emptying and motility)2, 5
Appropriate for nausea and vomiting caused by gastroparesis, functional bowel obstruction (due to opioid use) and gastro-oesophageal reflux disease2 |
Patients not currently receiving an antiemetic:
10 mg, subcutaneously every six hours, as needed (maximum dose 40 mg/24 hours)
Patients already receiving oral metoclopramide should be switched to:
10 mg, subcutaneously three to four times daily, as needed
OR
30 – 60 mg/24 hours, via CSCI8 however, in practice, patients whose symptoms are not adequately controlled with 40 mg metoclopramide, over 24 hours should be switched to levomepromazine
N.B Higher doses of metoclopramide, e.g. 60 mg over a 24-hour period, should be reserved for managing nausea and vomiting that is likely caused by delayed gastric emptying (without obstruction) |
Contraindicated in Parkinson’s disease, prolonged QT-interval, or if complete bowel obstruction10, 20
Monitor for extrapyramidal adverse effects, e.g. tardive dyskinesia (more common at doses greater than 30 mg/24 hours)
May worsen abdominal cramps in some patients
Do not co-prescribe with anticholinergics (e.g. cyclizine, hyoscine butylbromide) if delayed gastric emptying is the clear cause of nausea and vomiting3 |
5 mg/mL solution for injection (2 mL ampoules)
PSO and prescription |
Cyclizine*
H1 receptor antagonist with anticholinergic actions (at vomiting centre [NTS] and vestibular system)2
Recommended for nausea and vomiting resulting from raised intracranial pressure (due to brain tumours or secondary metastases), bowel obstruction and vestibular disease16 |
75 – 150 mg/24 hours, via CSCI16 |
Do not co-prescribe with metoclopramide if the likely cause of nausea and vomiting is delayed gastric emptying (without obstruction)3
Not recommended to be given as a subcutaneous bolus due to injection site reactions |
50 mg/mL solution for injection (1 mL ampoules)
PSO and prescription |
Levomepromazine (methotrimeprazine)†
Antagonistic action at dopamine, serotonin, cholinergic and histamine receptors18
Second-line, broad spectrum antiemetic16 |
3.125 – 6.25 mg, subcutaneously every four to six hours, as needed
OR
25 mg/24 hours8 |
Monitor for postural hypotension and excessive sedation18 |
25 mg/mL solution for injection (1 mL ampoules)
Only prescription** |
CSCI = continuous subcutaneous infusion
* Unapproved route
† Unapproved indication
** Three brands of levomepromazine injections are available on prescription: Levomepromazine (Wockhardt), Levomepromazin-Neuraxpharm (Section 29) and Nozinan (Section 29)
Acknowledgement
Thank you to the following experts for review of this article:
- Dr Kate Grundy, Palliative Medicine Physician, Clinical
Director of Palliative Care, Christchurch Hospital Palliative
Care Service and Clinical Lecturer, Christchurch School of
Medicine
- Vicki Telford, Clinical Nurse Specialist, Nurse Maude
Hospice Palliative Care Service, Christchurch
- Dr Helen Atkinson, General Practitioner and Medical
Officer, Harbour Hospice
- Dr Robert Odlin, General Practitioner, Orewa Medical
Centre
- Fraser Watson, Extended Care Paramedic Clinical Lead,
Hato Hone St John
N.B. Expert reviewers do not write the articles and are not responsible for the final content.
bpacnz retains editorial oversight of all content.
This resource is the subject of copyright which is owned by bpacnz.
You may access it, but you may not reproduce it or any part of it except in the limited situations described in the
terms of use on our website.
Article supported by Te Aho o Te Kahu, Cancer Control Agency.

References
- Ministry of Health – Manatū Hauora. Te Ara Whakapiri Toolkit: care in the last days of life. 2017. Available from: https://www.health.govt.nz/system/files/documents/publications/te-ara-whakapiri-toolkit-apr17.pdf (Accessed September, 2023).
- Moorthy GS, Letizia M. The management of nausea at the end of life. J Hosp Palliat Nurs 2018;20:442–9. https://doi.org/10.1097/NJH.0000000000000453
- NHS Scotland. Scottish palliative care guidelines - Nausea and vomiting. 2021. Available from: https://www.palliativecareguidelines.scot.nhs.uk/guidelines/symptom-control/Nausea-and-Vomiting.aspx (Accessed September, 2023).
- Leach C. Nausea and vomiting in palliative care. Clin Med 2019;19:299–301. https://doi.org/10.7861/clinmedicine.19-4-299
- Singh P, Yoon SS, Kuo B. Nausea: a review of pathophysiology and therapeutics. Therap Adv Gastroenterol 2016;9:98–112. https://doi.org/10.1177/1756283X15618131
- Zhong W, Shahbaz O, Teskey G, et al. Mechanisms of nausea and vomiting: current knowledge and recent advances in intracellular emetic signaling systems. IJMS 2021;22:5797. https://doi.org/10.3390/ijms22115797
- Lang IM. Physiology of the digestive tract correlates of vomiting. J Neurogastroenterol Motil 2023;29:20–30. https://doi.org/10.5056/jnm22105
- South Island Palliative Care Workstream. Te Ara Whakapiri Symptom management in the last days of life. 2020. Available from: https://www.sialliance.health.nz/wp-content/uploads/Symptom-management-in-the-last-days-of-life_SIAPO.pdf (Accessed September, 2023).
- Peralta T, Castel-Branco MM, Reis-Pina P, et al. Prescription trends at the end of life in a palliative care unit: observational study. BMC Palliat Care 2022;21:65. https://doi.org/10.1186/s12904-022-00954-z
- MacLeod R, Macfarlane S. The palliative care handbook. 9th ed. 2019. Available from: https://www.hospice.org.nz/wp-content/uploads/2019/03/Palliative-Care-Handbook.pdf (Accessed September, 2023).
- NHS Scotland. Scottish palliative care guidelines - Constipation. 2022. Available from: https://www.palliativecareguidelines.scot.nhs.uk/guidelines/symptom-control/Constipation.aspx (Accessed September, 2023).
- Roila F, Molassiotis A, Herrstedt J, et al. 2016 MASCC and ESMO guideline update for the prevention of chemotherapy- and radiotherapy-induced nausea and vomiting and of nausea and vomiting in advanced cancer patients. Annals of Oncology 2016;27:v119–33. https://doi.org/10.1093/annonc/mdw270
- Crawford GB, Dzierżanowski T, Hauser K, et al. Care of the adult cancer patient at the end of life: ESMO Clinical Practice Guidelines. ESMO Open 2021;6:100225. https://doi.org/10.1016/j.esmoop.2021.100225
- NHS Scotland. Scottish palliative care guidelines - Care in the last days of life. 2020. Available from: https://www.palliativecareguidelines.scot.nhs.uk/guidelines/end-of-life-care/Care-in-the-Last-Days-of-Life.aspx (Accessed September, 2023).
- Koia JH, Shepherd P. The potential of anti-diabetic rākau rongoā (Māori herbal medicine) to treat type 2 diabetes mellitus (T2DM) rate huka: a review. Front Pharmacol 2020;11:935. https://doi.org/10.3389/fphar.2020.00935
- New Zealand Formulary (NZF). NZF v135. Available from: www.nzf.org.nz (Accessed September, 2023).
- Mitchell K, Pickard J, Herbert A, et al. Incidence and causes for syringe driver site reactions in palliative care: a prospective hospice-based study. Palliat Med 2012;26:979–85. https://doi.org/10.1177/0269216311428096
- Cox L, Darvill E, Dorman S. Levomepromazine for nausea and vomiting in palliative care. Cochrane Database of Systematic Reviews 2015;2017. https://doi.org/10.1002/14651858.CD009420
- Prasad S, Katta MR, Abhishek S, et al. Recent advances in Lewy body dementia: a comprehensive review. Disease-a-Month 2023;69:101441. https://doi.org/10.1016/j.disamonth.2022.101441
- Chapman L, Ellershaw J. Care in the last hours and days of life. Medicine 2020;48:52–6. https://doi.org/10.1016/j.mpmed.2019.10.006





