Published: 17 June 2022 | Updated: 28 February 2024
What's changed?
28 February 2024 Update box added on 2023 NZ heart failure position statement
31 August 2023 update box on the four pillars of heart failure treatment added
27 June 2023 Ramipril added to Table 1
26 May 2023 Updated information on managing patients with HFpEF based on new American College of Cardiology 2023 guidelines
12 July 2022 Updated to include information from the 2022 AHA/ACC/HFSA (US) Heart Failure guideline which states that an ARNI, ACE inhibitor or ARB are all now equal first-line options for patients with heart failure
Key practice points:
- Following clinical diagnosis, pharmacological treatment for patients with heart failure should immediately proceed under the assumption they have reduced left ventricular ejection fraction (HFrEF); in general, this initially involves:
- Assertive treatment with a loop diuretic if the patient has fluid overload
- Initiation of an ACE inhibitor (or ARB) as soon as practically possible, and a beta-blocker once any symptoms of fluid overload have settled; these should subsequently be titrated to the maximum dose tolerated
- Spironolactone (or eplerenone) can be considered if patients remain symptomatic; in some patients with severe symptoms, spironolactone may be used concomitantly alongside the ACE inhibitor and beta-blocker immediately
- The combination product of valsartan (an ARB) and sacubitril (a neprilysin inhibitor) – class name ARNI; brand name Entresto – can also improve clinical outcomes in patients with ongoing symptomatic HFrEF despite optimised standard treatment (N.B. Some recent international guidelines, e.g. the 2022 AHA/ACC/HFSA (US) Heart Failure guideline, consider that an ARNI, ACE inhibitor or ARB are all now equal first-line options)
- Sacubitril + valsartan is fully funded with Special Authority approval
- Stop the patient’s ACE inhibitor (or ARB) before initiating sacubitril + valsartan due to the risk of angioedema
- There is increasing evidence that sodium-glucose cotransporter-2 (SGLT-2) inhibitors can improve prognostic outcomes in patients with heart failure, with or without diabetes. However, this medicine is currently only funded for patients with type 2 diabetes who meet the Special Authority criteria.
- If heart failure with preserved ejection fraction (HFpEF) is confirmed based on echocardiography at any point, a cardiologist should generally be involved to refine treatment, which mostly focuses on control of fluid balance using diuretics at the lowest possible dose, in addition to managing associated co-morbidities
Once heart failure has been diagnosed, pharmacological treatment needs to be initiated as soon as practically possible:1
 The short-term goal is to improve the patient’s symptoms/signs, and to reduce the risk of hospital admission
The short-term goal is to improve the patient’s symptoms/signs, and to reduce the risk of hospital admission
 The longer-term objective is to slow or prevent progressive deterioration of heart failure, thereby improving patient longevity
The longer-term objective is to slow or prevent progressive deterioration of heart failure, thereby improving patient longevity
In patients with an acute onset of significant heart failure symptoms, immediate hospital admission may be required where initial decisions regarding treatment will be made.1 However, in patients with a more gradual onset of symptoms, the process can begin in primary care. In this scenario, it is unlikely that echocardiography will have been performed yet, and therefore and it will not be known whether the patient has heart failure with reduced ejection fraction (HFrEF; i.e. signs/symptoms of heart failure and a left ventricular ejection fraction [LVEF] of less than 50%), or heart failure with preserved ejection fraction (HFpEF).
For further information on the terminology associated with heart failure, see: Part 1 – identifying and diagnosing heart failure
Proceed assuming the patient has HFrEF. Given that most evidence regarding effective management relates to patients with HFrEF, it is practical to initiate treatment in primary care assuming they have this subtype (Figure 1), and then modify the approach later on if echocardiology proves otherwise (see: “Treatment of patients with heart failure with a preserved ejection fraction (HFpEF)”).1

Figure 1. An overview of management for patients with heart failure with reduced ejection fraction (HFrEF) in primary care.1 HFrEF refers to patients with symptoms and signs of heart failure and a LVEF less than 50% confirmed by echocardiography. This algorithm can also be applied to patients with an undifferentiated clinical diagnosis of heart failure (i.e. echocardiography results are not yet available). See main text for more further information on treatment and monitoring requirements associated with each medicine.
* If a patient with heart failure has severe symptoms at presentation, they can potentially be cautiously initiated on an ACE inhibitor, beta blocker and spironolactone (i.e. at the same time) according to clinical judgement. However, a beta blocker should not be used unless the patient is euvolemic, and more frequent initial monitoring would be required (see: “Initiate an ACE inhibitor and a beta-blocker as soon as practically possible” and “Monitoring the effectiveness of treatment”).
N.B. The approach of using an ACE inhibitor first-line before trialling an ARB (if the ACE inhibitor is contraindicated or not tolerated) is consistent with 2018 National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand Heart Failure guidelines. However, in the 2022 AHA/ACC/HFSA Heart Failure guidelines from the United States ACE inhibitors, ARBs and ARNIs are all now considered first-line options. It is possible that New Zealand guidance may change over time.
Abbreviations: ACE inhibitor, angiotensin converting enzyme inhibitor; ARB, angiotensin receptor blockers; ARNI, angiotensin receptor II blocker with a neprilysin inhibitor; LVEF, left ventricular ejection fraction; SGLT-2 inhibitor, Sodium glucose co-transporter-2 inhibitor.
 Immediately prescribe a loop diuretic if the patient has fluid overload
Immediately prescribe a loop diuretic if the patient has fluid overload
Patients with symptomatic heart failure often have presenting features such as shortness of breath, elevated jugular venous pressure, bibasilar crackles or peripheral oedema – all of which are caused by hypervolaemia (fluid overload).2 Persisting hypervolaemia is a prognostic marker for poor survival in patients with heart failure.2
Immediate and assertive treatment with a loop diuretic such as furosemide is therefore a first priority for managing patients with heart failure and fluid overload:1, 3
- Initially 20 – 40 mg daily
- For resistant fluid overload, up-titrate in 20 – 40 mg increments to the minimum dose that improves symptoms and achieves weight loss of approximately 1 kg/day with a return to dry body weight
- The frequency of up-titration will depend on patient response and the severity of fluid overload (weekly is common)
- The usual dose range is 40 – 240 mg daily
Patients should initially be weighed and a “dry weight” target* established to progressively evaluate the effectiveness of diuresis. Blood pressure, serum potassium and renal function should also be measured throughout treatment, and urine output assessed.1 This titration protocol will be driven by the clinician in the short-term, however, some patients can make self-adjustments to diuretic dosing as required based on re-emerging symptoms in the longer-term. Patients should be informed that diuretic treatment should not continue long-term unless they are symptomatic; dosing should ideally be tapered over time as control is achieved with other medicine use.1
* Dry weight is the patient’s recorded/reported average weight before they began experiencing symptoms/signs of fluid overload.
Practice point: following the acute treatment period, discuss a heart failure action plan with the patient, which includes daily self-monitoring of changes in weight, swelling and shortness of breath. This can facilitate better self-management and treatment adherence, as well as prompt identification of symptom recurrence. For more information, see: https://assets.heartfoundation.org.nz/documents/heart-healthcare/heart-failure/heart-failure-action-plan.pdf?mtime=1667526701?1713320169
If furosemide is contraindicated or ineffective, a thiazide diuretic may be considered as an alternative or an add-on, however, these are contraindicated in patients with poor renal function (e.g. Stage IV chronic kidney disease or eGFR <30 mL/min/1.73 m2) and require more frequent monitoring.1
 Initiate an ACE inhibitor and a beta-blocker as soon as practically possible
Initiate an ACE inhibitor and a beta-blocker as soon as practically possible
ACE inhibitors and beta-blockers have been consistently demonstrated to reduce symptom severity and mortality in patients with HFrEF.1 These medicines have wide-ranging effects, such as directly reducing adverse left ventricular re-modelling and improving the ejection fraction, in addition to anti-arrhythmic and systemic blood pressure lowering effects.4
Medicine selection. Any ACE inhibitor is suitable as the beneficial effect is considered to be class-wide (N.B. funded access to cilazapril is restricted to existing patients only). The beta-blockers shown to improve outcomes for patients with HFrEF are carvedilol, bisoprolol and metoprolol succinate (the choice of which will be guided by patient specific factors).1
Treatment regimen. Both types of medicine should be prescribed to patients as soon as practically possible, however, recommendations in guidelines vary regarding the exact timing. In general:1
- An ACE inhibitor may be initiated at the same time as the diuretic
- Beta-blockers should be withheld until any symptoms of acute fluid overload have resolved (if present)
The general treatment approach is to start at a low dose and up-titrate to the maximum tolerated or specified dose (Table 1).1 If an ACE inhibitor is not tolerated, an angiotensin-II receptor blocker (ARB) such as losartan may be used.1 (see: “Does an ACE inhibitor always need to be initiated first?”). For some patients, beta-blocker up-titration needs to be more gradual to reduce the risk of adverse effects, and it can take longer to observe a change in symptoms.5
Does an ACE inhibitor always need to be initiated first?
Inhibition of the renin-angiotensin system is important to improve morbidity and mortality in patients with heart failure.5 However, there have been changes over time within the international literature regarding how to prioritise the different medicines affecting this system, i.e. ACE inhibitors, ARBs or angiotensin receptor II blocker with a neprilysin inhibitor (ARNI); for further information on ARNIs, see: “Angiotensin receptor-neprilysin inhibitor (ARNI)”.
For example:
- Australasian guidance: the 2018 National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand Heart Failure guideline recommends that an ACE inhibitor should be considered the first-line option. If an ACE inhibitor is contraindicated or not tolerated, an ARB can be used. Treatment can then be escalated by prescribing an ARNI as a replacement for an ACE inhibitor or ARB if patients with HFrEF remain symptomatic despite maximally tolerated treatment with an ACE inhibitor (or ARB) and a beta blocker (unless contraindicated) – provided they meet the Special Authority criteria.
- United States guidance: the 2022 AHA/ACC/HFSA Heart Failure guideline states that ACE inhibitors, ARBs and ARNIs are all now considered to be first-line options. ARBs are recommended in patients with intolerable cough, and as a preferable alternative to both ACE inhibitors and ARNIs in those with a history of angioedema. ACE inhibitors are noted as being less likely to cause hypotension than an ARNI so may benefit patients where this is a risk (N.B. this guidance presumably also applies to ARBs). This guideline also recommends that “if patients have chronic symptomatic HFrEF with NYHA class II or III symptoms and they tolerate an ACE inhibitor or ARB, they should be switched to an ARNI because of improvement in morbidity and mortality” and that “although data are limited, the use of an ARNI may be efficacious as de novo treatment in patients with symptomatic chronic HFrEF to simplify management”.
It is possible that New Zealand guidance relating to these medicines, and funding restrictions around the use of ARNIs, may change over time. ARBs are being increasingly used in New Zealand for the treatment of cardiovascular diseases, and many patients find them to be more tolerable than ACE inhibitors. If a patient is already taking an ARB (e.g. for pre-existing hypertension) then there is no recommendation they switch to an ACE inhibitor following a diagnosis of heart failure.
Table 1. Recommendations for ACE inhibitor, ARB and beta-blocker use in patients with heart failure.1, 3, 5, 6
|
ACE inhibitor* |
ARB |
Beta blocker |
Options |
Enalapril |
Lisinopril |
Quinapril |
Perindopril |
Ramipril‡ |
Candesartan |
Losartan |
Carvedilol |
Bisoprolol |
Metoprolol succinate (modified release) |
Starting dose† |
2.5 mg,
once daily |
2.5 mg,
once daily |
2.5 mg,
twice daily |
2 mg,
once daily |
1.25 mg,
once daily |
4 mg,
once daily |
12.5 mg,
once daily |
3.125 mg, twice daily |
1.25 mg, once daily |
23.75 mg, once daily |
Up-titration |
A gradual increase to maintenance dose is recommended. Check the NZF for medicine-specific up-titration recommendations but in general, double the dose no sooner than every two to four weeks up to the maximum tolerated or specified maintenance dose |
Usual maintenance dose
(otherwise aim for highest tolerated dose if this cannot be reached)† |
Usually 10 mg, twice daily (or 20 mg, once daily, if tolerated); higher doses, e.g. up to 20 mg, twice daily (or 40 mg, once daily, if tolerated), may be indicated in some patients, e.g. those with co-existing hypertension |
20 – 35 mg, once daily |
Usually 10 mg, twice daily (or 20 mg, once daily, if tolerated); higher doses, e.g. 20 mg, twice daily (or 40 mg, once daily, if tolerated), may be indicated in some patients, e.g. those with co-existing hypertension |
4 mg, once daily |
10 mg daily, preferably taken in two divided doses |
32 mg,
once daily |
150 mg,
once daily |
Highest tolerated dose up to a maximum of 25 mg, twice daily, in patients with severe heart failure or a body weight < 85 kg (may increase up to 50 mg, twice daily, if tolerated if the patient is > 85 kg) |
Highest tolerated dose up to a maximum of 10 mg, once daily |
Highest tolerated dose up to a maximum of 190 mg, once daily |
Initiate only if |
- Blood pressure is ≥ 100 mmHg systolic
- Potassium is < 5.5 mmol/L; significant caution is still required between 5.0 – 5.5 mmol/L
- Creatinine is < 250 micromol/L or eGFR is ≥ 30 ml/min/1.73 m2 (seek cardiologist advice if not)
|
- Symptoms of fluid overload have resolved and there are no symptoms of worsening heart failure
- No symptomatic bradycardia, hypotension or second- or third-degree heart block
|
Key short-term monitoring requirements |
- Check serum potassium and creatinine** one week after first dose
- Check blood pressure, serum potassium and creatinine prior to each dose increase; delay dose increase or seek cardiologist advice if blood pressure is < 95 mmHg, serum potassium is > 5.5 mmol/L or creatinine is > 25% above baseline
- Physical examination: weight, pulse, jugular venous pressure, chest auscultation
|
Long-term monitoring |
- Once stable dosing is achieved, continue long-term and monitor every three months (or more frequently if required depending on the patient)
|
Notes |
In general, discontinue potassium-supplements and potassium-sparing diuretics before introducing an ACE inhibitor; however, low dose mineralocorticoid receptor antagonists (e.g. spironolactone) may be used for heart failure if serum potassium is closely monitored |
If the patient has first degree heart block (i.e. PR interval > 0.2 seconds), an ECG is recommended before each dose increase. If an ECG is not available, seek cardiology advice |
* These are examples of ACE inhibitors with an approved indication for the treatment of patients with heart failure, but other ACE inhibitors can also be used as the beneficial effect is considered to be class-wide. N.B. cilazapril is no longer funded for new patients in New Zealand. For further information on prescribing ACE inhibitors, see:
bpac.org.nz/2021/ace.aspx. N.B. While the approach of trialling an ACE inhibitor before an ARB is consistent with 2018 New Zealand guidelines,5 some more recent international guidelines state that an ACE, ARB or ARNI are all considered equal first-line choices.
† For specific dosing information refer to the NZ Formulary (NZF) at nzf.org.nz. In some cases, cardiologists may recommend slightly different dosing regimens, or general practitioners may decide on a different regimen depending on patient-specific factors.
** An increase in serum creatinine of up to 30% above baseline is acceptable following initiation of an ACE inhibitor assuming it does not exceed 250 micromol/L; subsequent up-titrations should only occur if the creatinine increase is ≤ 25% above baseline (otherwise seek cardiologist advice).
‡ Ramipril doses listed are for patients with heart failure without previous myocardial infarction (unapproved indication). Dosing recommendations differ for patients with heart failure post-myocardial infarction (approved indication), however, treatment will likely be initiated and supervised in hospital – refer to the NZF at nzf.org.nz/nzf_1286 for further information.
Monitoring the effectiveness of treatment
Short-term. Patients with newly diagnosed heart failure who do not require hospitalisation should initially be reviewed at least weekly.7 Key monitoring requirements include medicine-specific adverse effects, changes in symptoms, clinical signs and exercise tolerance, as well as routine blood tests, e.g. electrolytes, renal function.7
Long-term. As symptoms improve, the monitoring frequency can be reduced; some patients with stable heart failure can be reviewed every three to six months in primary care.7 However, certain patients may require more frequent follow up, e.g. those who are frail or who are at an increased risk of decompensation.
 Repeat echocardiology is recommended to assess structural and functional cardiac changes in the long-term for patients receiving treatment, e.g. three months after medicine titration.1, 8 The patient’s LVEF should ideally remain > 40%. This approach will allow for further decisions regarding the use of advanced treatments (see: “Beyond primary care”), and further imaging may be considered based on the patient-specific symptoms and characteristics. N.B. While the frequency of echocardiology review should ideally depend on clear clinical indication, the timing of access may realistically be influenced by region-specific resource availability.
Repeat echocardiology is recommended to assess structural and functional cardiac changes in the long-term for patients receiving treatment, e.g. three months after medicine titration.1, 8 The patient’s LVEF should ideally remain > 40%. This approach will allow for further decisions regarding the use of advanced treatments (see: “Beyond primary care”), and further imaging may be considered based on the patient-specific symptoms and characteristics. N.B. While the frequency of echocardiology review should ideally depend on clear clinical indication, the timing of access may realistically be influenced by region-specific resource availability.
 If brain natriuretic peptide (BNP) levels were found to be substantially elevated at diagnosis, monitoring for a decrease in these levels may be considered as a further marker of treatment efficacy. However, serial measurements are not routinely recommended and decreases may not occur in all patients.7, 9 This approach is likely only suitable if it will influence management decisions, particularly if there is uncertainty about the cause of a change in symptoms, e.g. whether improvement in shortness of breath is due to the changing status of COPD or heart failure.
If brain natriuretic peptide (BNP) levels were found to be substantially elevated at diagnosis, monitoring for a decrease in these levels may be considered as a further marker of treatment efficacy. However, serial measurements are not routinely recommended and decreases may not occur in all patients.7, 9 This approach is likely only suitable if it will influence management decisions, particularly if there is uncertainty about the cause of a change in symptoms, e.g. whether improvement in shortness of breath is due to the changing status of COPD or heart failure.
N.B. BNP levels often rise during the first few weeks of beta-blocker treatment, before dropping with sustained use.7 If serial BNP testing is done for any reason, do not repeat tests within two weeks and ideally request no more than four tests per year.9
 Options for patients with resistant heart failure or more severe presentations
Options for patients with resistant heart failure or more severe presentations
Mineralocorticoid receptor antagonists
Spironolactone is a mineralocorticoid receptor antagonist recommended for patients with heart failure who remain symptomatic despite maximal doses of an ACE inhibitor/ARB and a beta-blocker, or for people with severe symptoms at presentation. In clinical trials, the use of these three medicines in combination decreases mortality by 50 – 60% over one to three years.1
Spironolactone may be initiated if the patient’s eGFR is > 30mL/min/1.73 m2 and their serum potassium is < 5.0 mmol/L.10 This medicine should be used with caution in patients with impaired renal function and may cause hyperkalaemia; creatinine and electrolytes should therefore be monitored regularly, i.e. at one week, one month and then at least six monthly.10
If spironolactone is not tolerated or the patient experiences significant anti-androgenic adverse effects, an alternative dose-equivalent mineralocorticoid receptor antagonist, eplerenone, can be prescribed with Special Authority approval, provided that the patient has a LVEF < 40%.3, 11 Eplerenone is associated with similar rates of cardiovascular protection compared with spironolactone, but has reduced rates of gynaecomastia or breast tenderness which are common reasons for treatment discontinuation in males taking a mineralocorticoid receptor antagonist.11
Angiotensin receptor-neprilysin inhibitor (ARNI)
Sacubitril + valsartan (Entresto) is the only available example in a new class of medicine combining an angiotensin receptor II blocker with a neprilysin inhibitor (ARNI; Figure 2). When taken concomitantly with a beta-blocker, ARNIs reduce the absolute risk of cardiovascular death or hospitalisation by almost 5% compared with an ACE inhibitor in patients with symptomatic heart failure.12 The original trial investigating sacubitril + valsartan (PARADIGM-HF) was stopped early after a median follow-up of 27 months due to the significant benefit associated with ARNI use versus ACE inhibitor treatment.12 The number need to treat (NNT) during the study to prevent one primary event (involving a composite of CV death or hospitalisation relating to heart failure) was estimated to be 21.12
N.B. While Australasian guidelines have previously recommended that an ARNI should not be used until either an ACE inhibitor or ARB has been trialled,5 the 2022 AHA/ACC/HFSA (US) Heart Failure guideline states that ACE inhibitors, ARBs and ARNIs are all now considered first-line options (see: “Does an ACE inhibitor always need to be initiated first?”).
A 2022 consensus statement from Australian clinicians also endorses the AHA/ACC/HFSA guideline approach, i.e. prioritising immediate or early ARNI use in patients with HFrEF. This shift lends support to the approach of using multiple evidence-based medicines early, rather than stepwise changes in accordance with patient symptoms, to promote optimal patient outcomes (see: “The four pillars of heart failure treatment”).
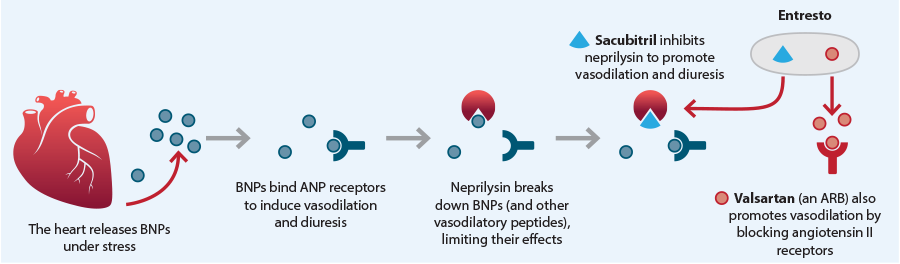
Figure 2. Mechanism of action for the ARNI sacubitril + valsartan (Entresto).13
Special Authority applications for sacubitril + valsartan can be made by any relevant practitioner for patients who have NYHA class II – IV symptoms and who are receiving concomitant optimal standard chronic heart failure treatments.3 The criteria state that patients should either have a confirmed LVEF < 35%, or if echocardiography is not practically possible the medicine can be initiated if the clinician believes they are “likely to benefit from treatment”.3 The Special Authority criteria may be subject to change over time – for the most recent information check the Special Authority form (see: https://schedule.pharmac.govt.nz/SAForms.php).
Sacubitril + valsartan should not be initiated until at least 36 hours after the last dose of ACE inhibitor or at least 24 hours after the last dose of ARB; this combination is contraindicated due to the elevated risk of angioedema.1 There are three strengths of sacubitril + valsartan available, each to be prescribed twice daily:3
- 24.3 mg sacubitril/25.7 mg valsartan (rounded to 24 mg/26 mg)
- 48.6 mg sacubitril /51.4 mg valsartan (rounded to 49 mg/51 mg)
- 97.2 mg sacubitril /102.8 mg valsartan (rounded to 97 mg/103 mg)
In general, patients can be initiated on the “medium” 49 mg/51 mg dose, and up-titrated to the “high” 97 mg/103 mg dose if tolerated. The “low” 24 mg/26 mg starting dose is reserved for high risk patient groups, e.g. those with hypotension, older or frail patients, those with severe renal or hepatic impairment.14
Blood pressure, renal function and serum potassium should be reviewed at initiation, with each dose increase, and every three to six months once the patient is stable (in the absence of relevant risk factors).14 If a patient’s systolic blood pressure is < 100 mmHg at initiation, delay use until this is resolved.14 The use of BNP as a biomarker for treatment efficacy is not routinely recommended as neprilysin inhibitors (e.g. sacubitril) prevent BNP-32 degradation; NT-proBNP (N-terminal proBNP) monitoring can be considered if necessary if this specific test is available at the local community laboratory.
Practice point: if hypotension occurs at any stage during sacubitril + valsartan treatment, this should ideally be addressed first by lowering the dose of any diuretic or other antihypertensive medicines. If hypotension persists, then a dose decrease of sacubitril + valsartan can be considered (or discontinued).13
 Additional medicines to consider based on patient co-morbidities
Additional medicines to consider based on patient co-morbidities
Digoxin. Consider digoxin if patients have heart failure associated with atrial fibrillation and symptoms cannot be adequately controlled with a beta-blocker.1 There is some evidence this medicine may improve symptoms and reduce the rate of hospitalisation, however, it does not improve survival.1 If digoxin is used, lower doses (e.g. 62.5 – 125 micrograms once daily) are generally recommended;3, 10 there is evidence that mortality is significantly higher in patients with serum levels ≥ 1.2 ng/ml.10
Anticoagulants. An anticoagulant should be considered in patients who have heart failure associated with atrial fibrillation who are at risk of stroke.1 The CHA2DS2-VASc is a recommended tool to assess stroke risk.
Intravenous iron. Anaemia is common in patients with heart failure and often occurs as a result of iron deficiency; other potential causes include vitamin B12 and folate deficiency or chronic kidney disease.1 Iron deficiency can also occur without anaemia.1 After addressing any reversible causes, e.g. blood loss, iron replacement should be considered for patients with heart failure who have serum ferritin levels < 100 micrograms/L, or serum ferritin levels 100 – 300 micrograms/L and transferrin saturation (TSAT) < 20%.15, 16 Conventional thresholds for diagnosing iron deficiency (usually serum ferritin ≤ 20 micrograms/L) are not reliable in patients with heart failure as this condition involves a systemic inflammatory state and ferritin levels become elevated in response to inflammation.17 Oral iron supplementation has been shown to have minimal benefit in such patients.1 Instead, administering intravenous iron is often preferred in patients with heart failure who are iron deficient and correction has been found to improve symptoms, exercise tolerance and reduce the risk of hospitalisation in clinical trials, as well as improve quality of life outcomes.1, 15
N.B. Ferric carboxymaltose (Ferinject) is suitable for administration in a primary care setting and is funded with Special Authority approval for patients with iron deficiency anaemia (i.e. low haemoglobin) with a serum ferritin of ≤ 20 micrograms/L, and oral iron treatment has proven ineffective or resulted in dose-limiting intolerance or rapid correction of anaemia is required.* Patients with iron deficiency alone are not currently eligible† for funded treatment, but some PHOs may offer funding for select patients.
* Applications under these criteria can be made by any relevant medical practitioner. A specialist, or any medical practitioner on recommendation from a specialist, can also apply for Special Authority approval if the patient has heart failure and iron deficiency anaemia without a specific serum ferritin threshold and “a trial of oral iron is unlikely to be effective”.
† Special Authority approval criteria may change over time. See the New Zealand Formulary or Special Authority form for the most recent criteria.
Sodium-glucose co-transporter-2 (SGLT-2) inhibitors. SGLT-2 inhibitors (e.g. empagliflozin) are highly effective for improving prognostic outcomes in patients with heart failure (see: “SGLT-2 inhibitors: a promising addition to the cardioprotection toolbox”),1, 18 and protect against the progression of proteinuric renal dysfunction in patients with chronic kidney disease.19 However, SGLT-2 inhibitors are currently only funded in New Zealand for patients with type 2 diabetes who have poor glycaemic control and are at high risk of cardiovascular disease.20
 Recommend a SGLT-2 inhibitor for patients with type 2 diabetes and heart failure who qualify for funded treatment – since 1 February 2021, empagliflozin is fully funded for patients with type 2 diabetes who meet Special Authority criteria. This includes all patients with type 2 diabetes with sub-optimal glycaemic control despite regular use of at least one blood-glucose lowering medicine, who are of Māori or Pacific ethnicity, or who have a high risk of or existing cardiovascular disease, or diabetic kidney disease.
Recommend a SGLT-2 inhibitor for patients with type 2 diabetes and heart failure who qualify for funded treatment – since 1 February 2021, empagliflozin is fully funded for patients with type 2 diabetes who meet Special Authority criteria. This includes all patients with type 2 diabetes with sub-optimal glycaemic control despite regular use of at least one blood-glucose lowering medicine, who are of Māori or Pacific ethnicity, or who have a high risk of or existing cardiovascular disease, or diabetic kidney disease.
For further information on SGLT-2 inhibitors and the full Special Authority criteria, see: bpac.org.nz/2021/diabetes.aspx
 Discuss the idea of patients self-funding a SGLT-2 inhibitor if they are not eligible for funded access, i.e. they do not have diabetes or do not meet the Special Authority criteria
Discuss the idea of patients self-funding a SGLT-2 inhibitor if they are not eligible for funded access, i.e. they do not have diabetes or do not meet the Special Authority criteria

SGLT-2 inhibitors: a promising addition to the cardioprotection toolbox
SGLT-2 inhibitors are an emerging treatment option for patients with heart failure even if they do not have type 2 diabetes. A meta-analysis of randomised placebo-controlled trials (N = 66,957) demonstrated that SGLT-2 inhibitors reduce the combined relative risk of cardiovascular death or hospitalisation by 24% in patients with heart failure compared with placebo.21 This cardioprotective benefit occurs for both patients with HFrEF and those with HFpEF, with or without diabetes.21
While the conventional approach to treatment (i.e. initial use of an ACE inhibitor/ARB plus a beta blocker) remains standard practice in New Zealand for patients with newly diagnosed heart failure, in part due to current funding criteria for medicines, the combination of an ARNI, beta blocker, mineralocorticoid receptor antagonist and SGLT-2 inhibitor (dubbed “comprehensive disease-modifying treatment”) has been estimated to:
- Reduce the relative risk of cardiovascular death or hospitalisation by 62% compared with standard treatment (i.e. ACE inhibitor/ARB and beta blocker)22
- Provide on average an additional five years of life for a patient aged 70 years with heart failure compared with no treatment23
The four pillars of heart failure treatment
International guidelines are increasingly recommending that most patients with heart failure should be established on the “four pillars of heart failure treatment” as early as possible, including an ARNI, beta blocker, MRA and SGLT-2 inhibitor (Figure 3A).a, b The practical capacity to achieve this combination of medicines will depend on patient co-morbidities and funding restrictions, but should be encouraged where possible to decrease mortality and hospitalisation (Figure 3B),c and potentially support cardiac structure recovery. Treatment can be initiated and optimised based on a clinical diagnosis of heart failure in primary care (i.e. there is no need to wait for echocardiography); the approach to management can be refined later, if required, once echocardiogram results are available.

Figure 3. (A) The four pillars of heart failure treatment.a, b (B) The risk of cardiovascular mortality or hospitalisation related
to heart failure in patients with HFrEF compared with ACE inhibitor treatment alone. Adapted from Tromp et al, 2022.c
- Straw S, McGinlay M, Witte KK. Four pillars of heart failure: contemporary pharmacological therapy for heart failure with reduced ejection fraction. Open
Heart 2021;8:e001585. doi:10.1136/openhrt-2021-001585
- Docherty KF, Bayes-Genis A, Butler J, et al. The four pillars of HFrEF therapy: is it time to treat heart failure regardless of ejection fraction? European Heart
Journal Supplements 2022;24:L10–9. doi:10.1093/eurheartjsupp/suac113
- Tromp J, Ouwerkerk W, Van Veldhuisen DJ, et al. A systematic review and network meta-analysis of pharmacological treatment of heart failure with reduced
ejection fraction. JACC: Heart Failure 2022;10:73–84. doi:10.1016/j.jchf.2021.09.004
Update: 2023 position statement on improving management for patients with heart failure in Aotearoa New Zealand
A position statement has been published by a collective of New Zealand cardiology experts (the Heart Failure Working Group), endorsed by the Cardiac Society of Australia and New Zealand (NZ Region), and the New Zealand Heart Foundation. This statement comes in response to developing perspectives around optimal heart failure management in local and international guidelines, as well as evidence that health inequities relating to heart failure continue to widen in New Zealand. A recent national study found that between 2006 and 2018, the incidence of hospitalisation for heart failure declined progressively for people of European/Other and Asian ethnicity, but did not decrease for Māori and Pacific peoples. In 2018, rates of hospitalisation related to heart failure were 6-fold higher for Māori and Pacific peoples compared with European/Others in those aged < 50 years, 3.5-fold higher in those aged 50 – 69 years and 1.5-fold higher in those aged ≥ 70 years.
The position statement recommends use of “the four pillars of heart failure treatment” – also known as guideline-directed medical therapy (GDMT) – as early as possible in all patients with HFrEF to improve clinical outcomes, i.e. an ARNI, beta blocker, MRA and SGLT-2 inhibitor. To better enable this approach, the Group recommends that sacubitril/valsartan, empagliflozin and eplerenone treatment should be fully funded without the need for Special Authority approval in patients with HFrEF. The statement also emphasises that while combined GDMT has not been associated with the same efficacy in RCTs involving patients with HFpEF, the potential benefits and recommendations for SGLT-2 inhibitor treatment should apply regardless of LVEF status.
For the full position statement, see: https://nzmj.org.nz/journal/vol-137-no-1590/2023-position-statement-on-improving-management-for-patients-with-heart-failure-in-aotearoa-new-zealand N.B. Individuals must subscribe and log in to view this resource, however, there is no subscription fee
There is minimal evidence regarding the effective treatment of patients with HFpEF. It is difficult – if not impossible – to differentiate this subtype based on clinical features alone. However, HFpEF generally affects older patients with multiple co-morbidities.1 If at any point echocardiography results demonstrate that the patient has HFpEF, seek the advice of a cardiologist who will guide initial treatment decisions.1
General principles of management for patients with HFpEF includes:1, 24
- Use of a loop diuretic at the lowest possible dose if the patient has fluid overload
- Management of co-morbidities, e.g. atrial fibrillation, ischaemic heart disease, hypertension, diabetes
- Use of ARBs (see update box) or beta blockers as required without the need to maximise the dose; diltiazem and verapamil can be considered as an alternative to beta-blockers for rate control (these are contraindicated in patients with HFrEF)
- ARNIs are a possible alternative to ARBs, however, patients may not be eligible for funded treatment (see update box)
- Mineralocorticoid receptor antagonists, e.g. spironolactone, can be considered to reduce the risk of hospitalisation
- SGLT-2 inhibitors for patients without contraindications (currently only funded for patients with concurrent type 2 diabetes; see update box)
The 2023 ACC guidelines highlight that while the prevalence of HFpEF is increasing, it remains under-recognised in daily practice and patients can present with a diverse range of co-morbidities, e.g. hypertension, diabetes, obesity.24 Primary care clinicians should consider HFpEF as a possible diagnosis in any patient presenting with dyspnoea (particularly if they are also obese), exercise intolerance and oedema.24 The symptom burden at presentation is often more severe in females with HFpEF compared with males.24
HFpEF is defined as signs/symptoms of heart failure in patients with a LVEF ≥ 50%, however, making a diagnosis also requires exclusion of:24
- Non-cardiac causes of symptoms/signs, e.g. lymphoedema, chronic kidney disease, liver disease, chronic venous insufficiency
- Cardiac mimics of HFpEF, e.g. hypertrophic cardiomyopathy, infiltrative cardiomyopathy, valvular heart disease, pericardial disease
There can also be further challenges during the diagnostic work-up. For example, BNP levels are often lower in people with HFpEF who are obese (and in some cases may be below diagnostic thresholds) and echocardiogram may not demonstrate obvious structural/functional cardiac abnormalities.24 To support the diagnostic evaluation, ACC guidelines recommend using scoring tools to estimate the likelihood of HFpEF, which can support decision-making in primary care prior to cardiology referral for confirmation.24 General practitioners may find the H2FPEF tool useful as this relies on clinical information readily accessible in primary care.24 HFA-PEFF is another tool but this may be less practical because it involves more in-depth testing information (e.g. BNP levels, echocardiogram results, diastolic stress testing) and specialised investigations (e.g. MRI/CT imaging, biopsy, genetic testing) that can be difficult to access in the community.24
The 2023 ACC guidelines re-emphasise the importance of managing co-morbidities in patients with HFpEF, in addition to non-pharmacological management strategies, e.g. exercise, weight loss.24 While medicine selection will vary between patients depending on underlying co-morbidities (and optimisation should be directed by a cardiologist), SGLT-2 inhibitors are now recommended in all patients with HFpEF without contraindications. Current Special Authority criteria for funded access to empagliflozin requires the patient to have a diagnosis of type 2 diabetes (in addition to other criteria).* Patients with HFpEF who do not have a diagnosis of diabetes may wish to consider self-funding. In addition, ACE inhibitor use is now discouraged in favour of an ARNI or ARB based on evidence for greater benefit in patients with a more preserved LVEF. In New Zealand, initial applications for Special Authority subsidy require patients to have either a confirmed LVEF <35%, or a heart failure diagnosis that is undifferentiated due to echocardiography being considered “not reasonably practical”.24* This may present a barrier to access to ARNIs for some patients.
* Criteria current as of May, 2023.
Lifestyle advice and education are important to improve the outcomes of pharmacological treatment in all patients with heart failure, regardless of the subtype.1
This includes:1, 15
- Understanding appropriate action to take if symptoms worsen
- Undertaking regular exercise as appropriate/tolerated
- Reducing daily sodium intake (preferably < 3 g daily; no more than 5 g daily).
Read the evidence
The SODIUM-HF trial demonstrated that a strict low sodium diet of < 1.5 g daily does not reduce the risk of a composite endpoint including cardiovascular-related admission to hospital, cardiovascular-related emergency department visit, or all-cause death in patients with heart failure compared with those receiving “general advice to restrict dietary sodium” (N.B. this comparator group is therefore still sodium restricted).25 However, modest improvements in patient-reported quality of life and clinician assessed NYHA functional class were identified in the low sodium group.25
- Weight loss if the patient is overweight
- Consuming an adequate but not excessive amount of fluid, e.g. 1.5 – 2 L daily (N.B. people with physically demanding jobs or who work outdoors may need to consume more fluid to compensate for water loss during the day)
- Reducing alcohol intake and smoking cessation, if relevant
- Encouraging influenza and pneumococcal vaccination (these infections can be a significant cause of decompensation); people with congestive heart failure are eligible for funded annual influenza vaccination
- Ensure patient is up to date with recommended COVID-19 vaccinations
Decompensation in previously stable patients
Episodes of acute deterioration (decompensation) can occur for various reasons in patients with heart failure who have previously been stable.15 Some patients are prone to recurrent episodes of decompensation despite ongoing treatment adherence.
A number of factors can result in decompensation, including:15
- Poor medicine adherence or changes to the patient’s regimen, e.g. reducing diuretic dose, adding a new medicine (including over-the-counter items, particularly NSAIDs)
- Uncontrolled hypertension
- Cardiac arrhythmia (most often atrial fibrillation)
- Cardiac ischaemia
- Cardiac infection or inflammation
- Systemic infection (secondary to increased haemodynamic demand on the heart)
- Changes in diet (primarily affecting sodium) and fluid intake
- Changes in exercise levels
- Physical or mental exhaustion
- Chronic right ventricular pacing
- Substance misuse
The journey for patients with heart failure can vary substantially. For patients who remain symptomatic despite optimal medicine use, or who require frequent secondary care involvement, additional options to improve survival include surgery or device management, e.g. with an implantable cardioverter defibrillator, cardiac resynchronisation therapy (CRT) or CRT-defibrillation.1
Consider referral to a cardiologist to discuss these advanced procedures for patients with:1
- LVEF persistently < 40%
- Valvular heart disease, or other forms of confirmed underlying cardiac pathology
- Heart failure and syncope – insertion of a pacemaker may be required
- Heart failure and left bundle branch block, with a wide QRS on ECG associated with ventricular dyssynchrony – CRT may be indicated
- A history of cardiac arrest or ventricular tachycardia – defibrillator therapy may be indicated
Despite advances in pharmacological, surgical and device interventions over time, almost 40% of patients diagnosed with heart failure do not survive longer than 12 months after their first hospitalisation.1 If patients with advanced heart failure continue to experience deteriorating and distressing symptoms despite treatment, the focus may need to shift from prevention of disease progression to improving quality of life outcomes in a palliative care setting. Given that this can be a confronting topic, it is important to introduce the concept as early as possible during a shared discussion between the patient, family/whānau or carer, cardiologist and primary care team.1 Through this approach, patients can progressively evaluate and convey when they feel the time is right to make this transition.
For further information on advance care planning, see: www.hqsc.govt.nz/our-programmes/advance-care-planning/





